Lots of interesting abstracts and cases were submitted for TCTAP 2026. Below are the accepted ones after a thorough review by our official reviewers. Don’t miss the opportunity to expand your knowledge!
CASE20251112_003
When One Vessel Holds It All: Navigating a Challenging Primary PCI in Single Coronary Circulation
By Deri Arara, Billal Patel, Mohammad Ezam Emran
Presenter
Deri Arara
Authors
Deri Arara1, Billal Patel1, Mohammad Ezam Emran1
Affiliation
Gleneagles JPMC, Brunei Darussalam1
View Study Report
CASE20251112_003
Coronary - ACS/AMI
When One Vessel Holds It All: Navigating a Challenging Primary PCI in Single Coronary Circulation
Deri Arara1, Billal Patel1, Mohammad Ezam Emran1
Gleneagles JPMC, Brunei Darussalam1
Clinical Information
Relevant Clinical History and Physical Exam
A 54-year-old woman presented with worsening chest pain for seven days. She denied palpitations or dyspnea. Two months earlier, she was hospitalized for NSTEMI, and angiography showed severe two-vessel disease with an anomalous RCA arising from the mid-LAD. CABG was planned but not completed due defaulted follow up. On current admission, BP was 135/78 mmHg, HR 80 bpm, with clear lungs and no cardiac murmurs.

Relevant Test Results Prior to Catheterization
A 54-year-old woman presented with worsening chest pain for seven days. She denied palpitations or dyspnea. Two months earlier, she was hospitalized for NSTEMI, and angiography showed severe two-vessel disease with an anomalous RCA arising from the mid-LAD. CABG was planned but patient defaulted to follow-up. On current admission, BP was 135/78mmHg, HR 80 bpm, with clear lungs and no cardiac murmurs.
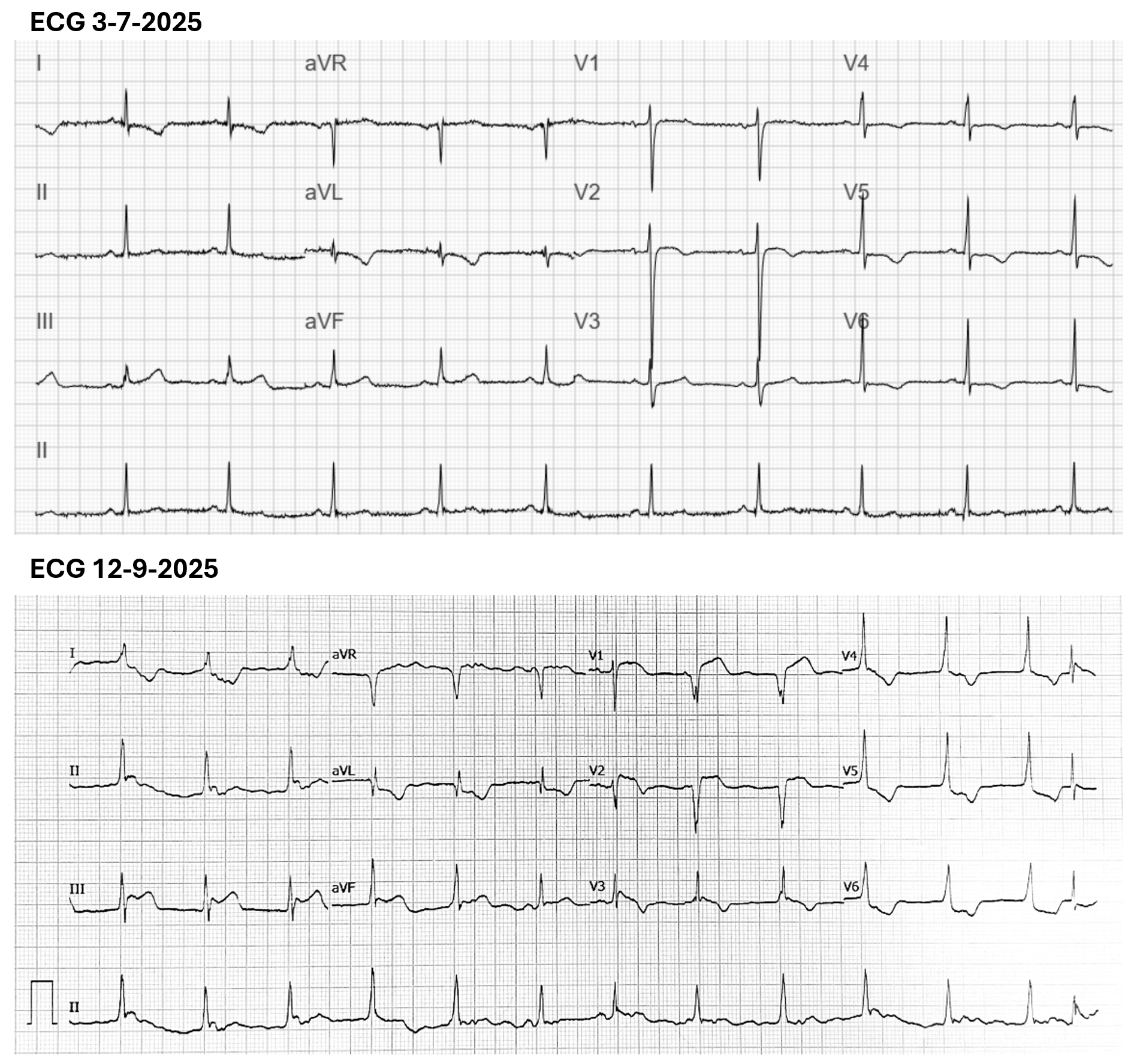
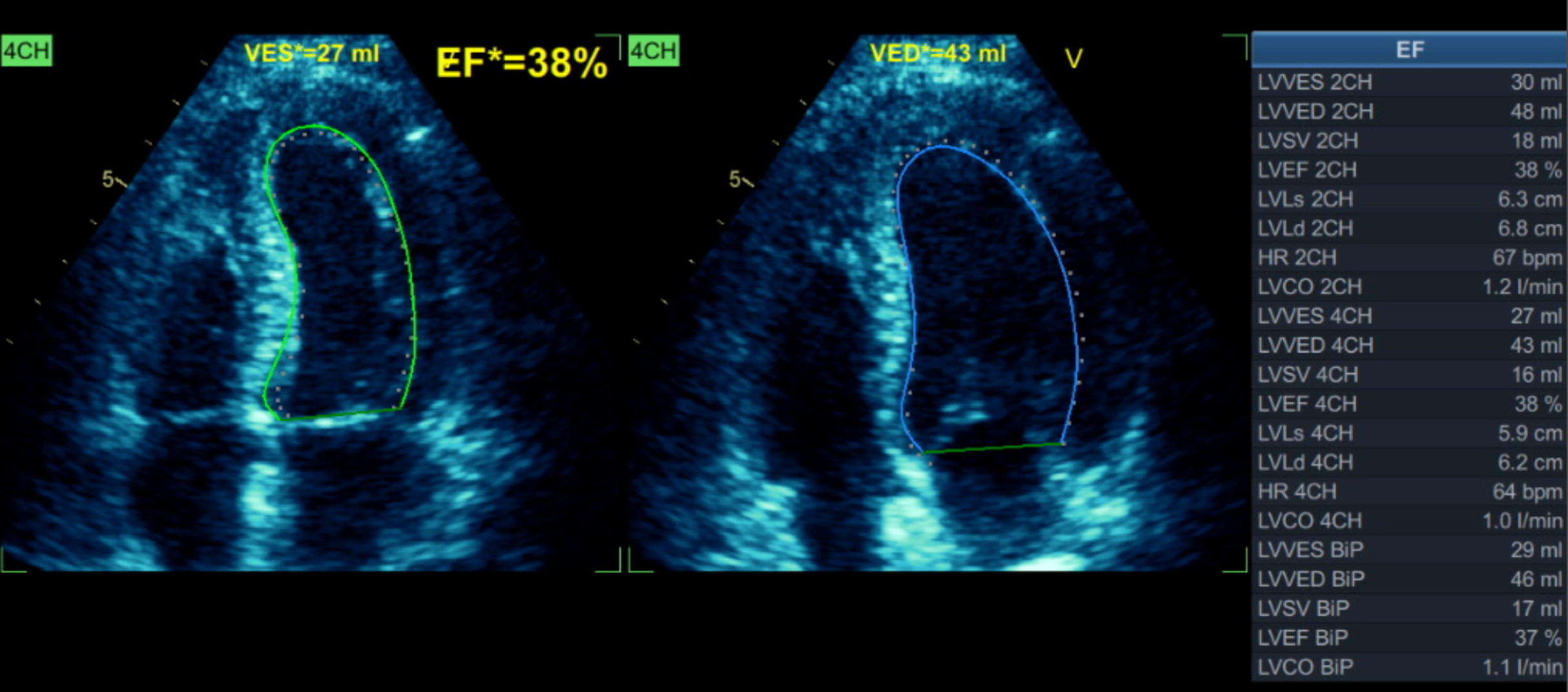
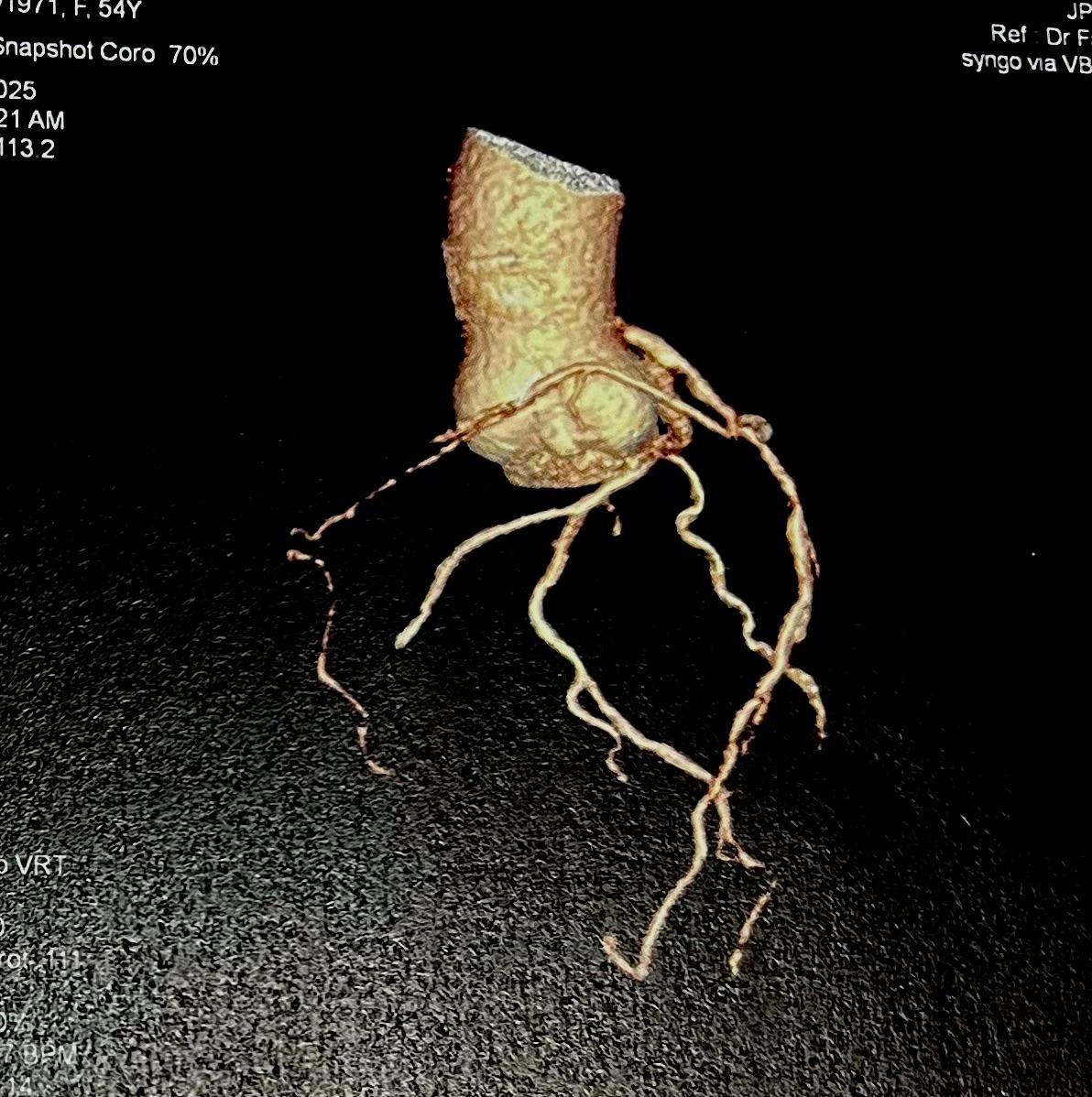



Relevant Catheterization Findings
The initial angiogram on July 3rd, 2025, showed two-vessel coronary artery disease, with diffuse atherosclerosis extending from the proximal to distal LAD and moderate stenosis of the OM2. The RCA was absent and appeared to be supplied by the D1 branch, which showed severe disease at the ostium and mid segment. A repeat angiogram showed drop of blood flow with TIMI 2 flow to the distal LAD and RCAterritories. Then we proceed to PCI to LAD and RCA.
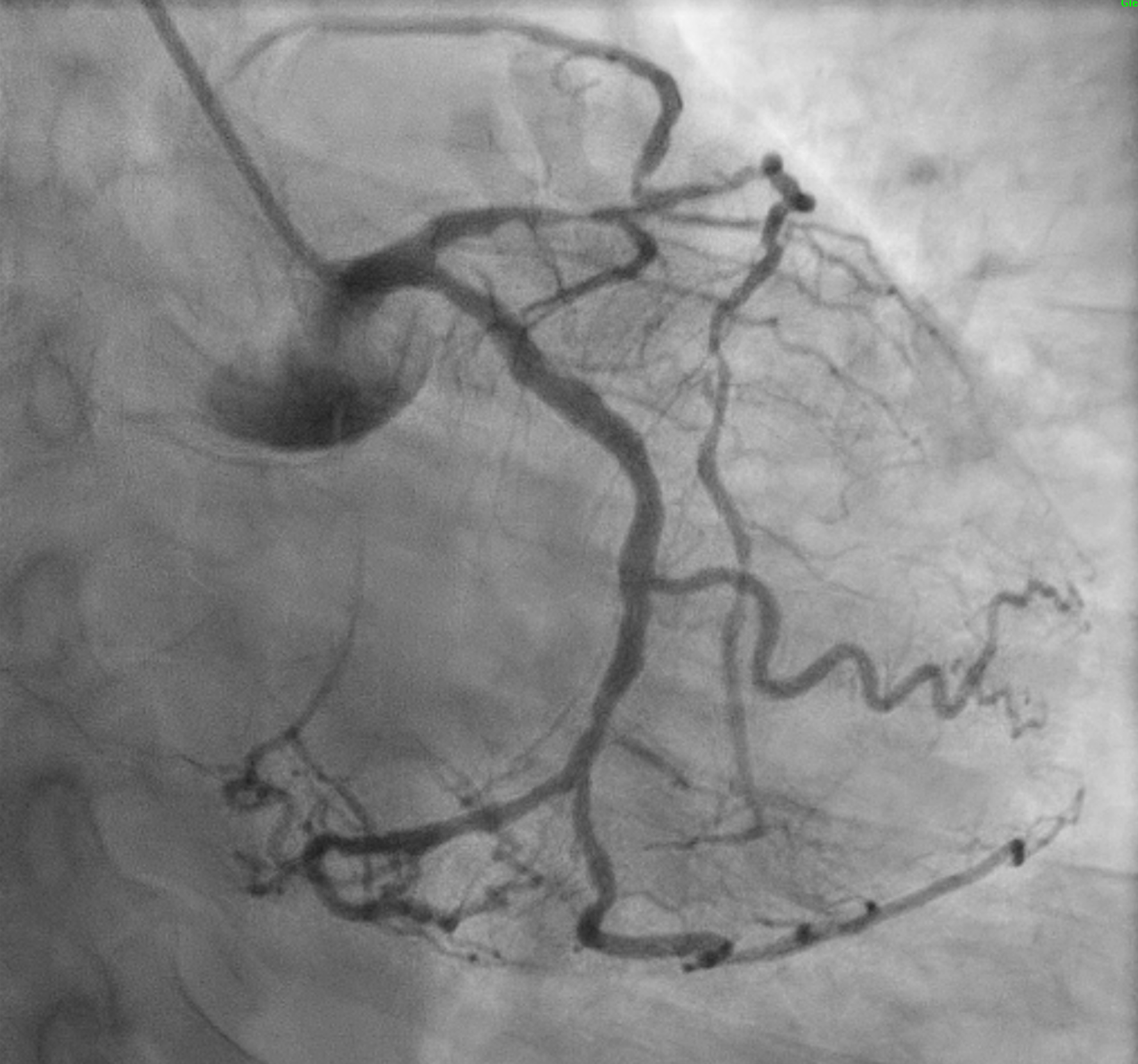
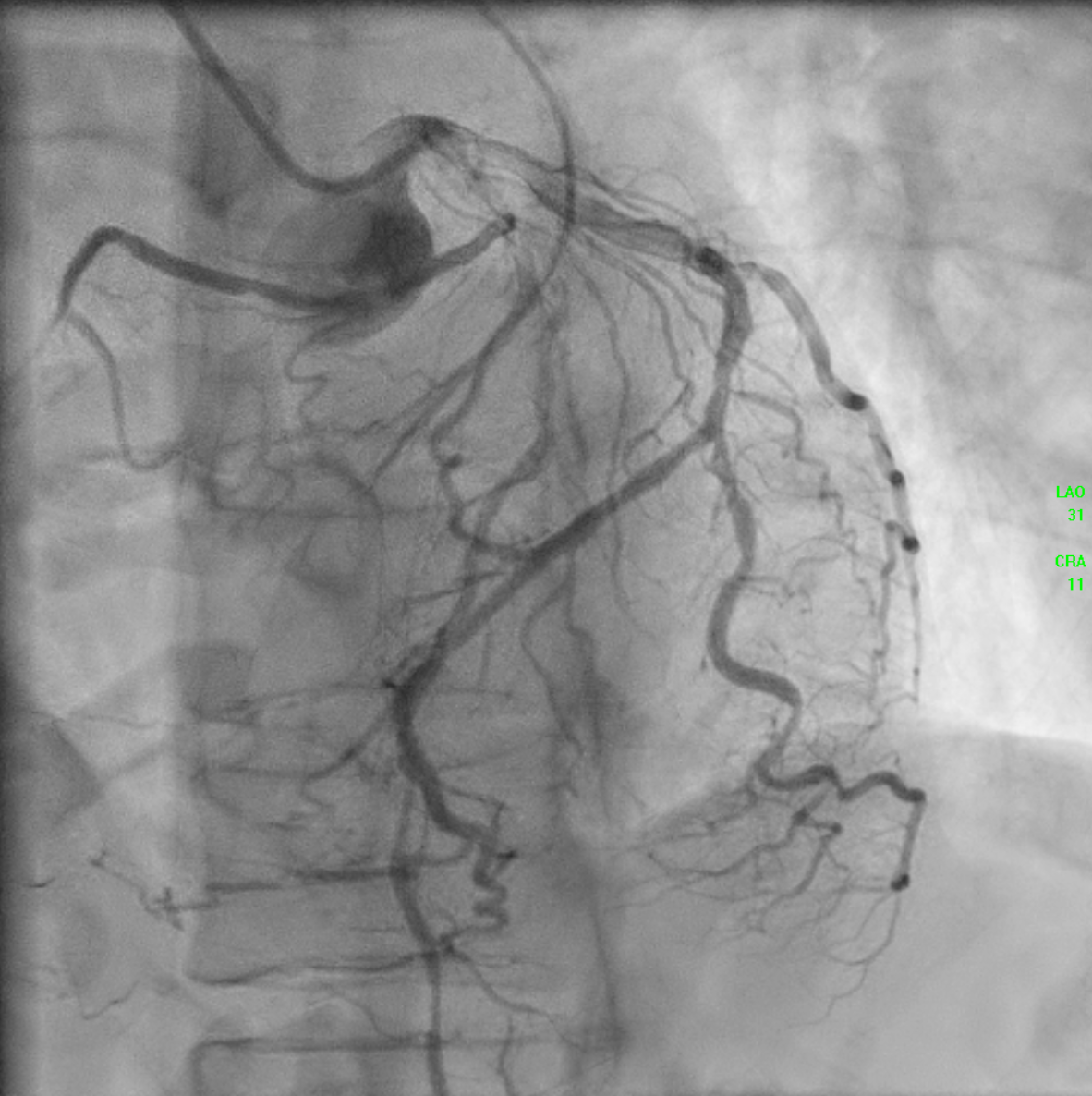
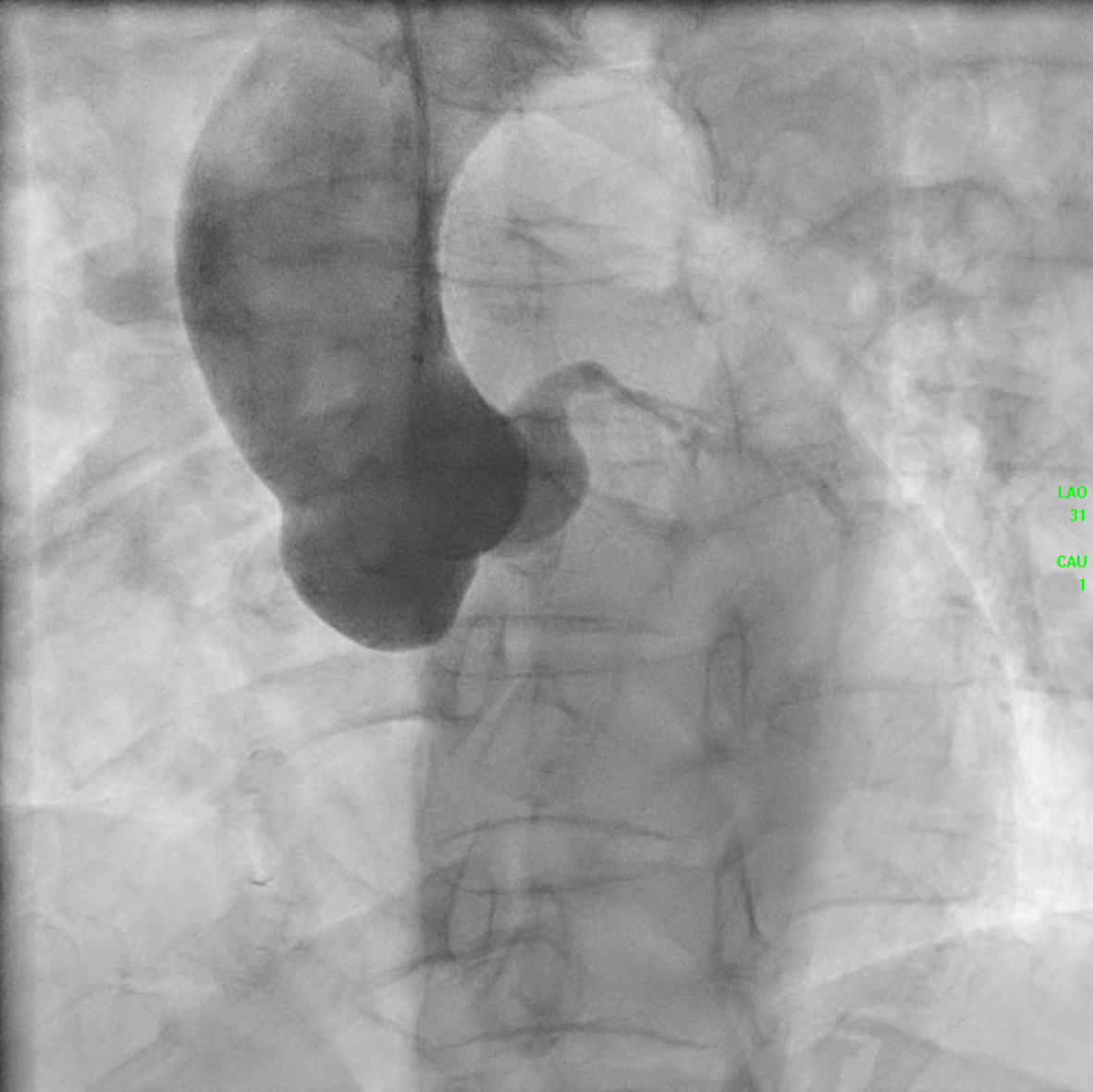
 AORTOGRAM.mp4
AORTOGRAM.mp4
 PA-CAU.mp4
PA-CAU.mp4
 PA-CRA + SPIDER.mp4
PA-CRA + SPIDER.mp4



Interventional Management
Procedural Step
An IVUS-guided PCI of the LAD and RCA was performed via right radial access. An EBU 3.5, 7 Fr guiding catheter engaged the left main, and a Sion Blue wire was advanced to the distal LAD for pre-dilatation with a 2.5 mm NC balloon. Wiring the anomalous RCA from the LAD was challenging due to a retroflexed ostium but was achieved using a reverse wire technique with adual-lumen (Sasuke) catheter and Sion Black wire. Difficulty crossing the mid RCA, likely due to dissection, required multiple wire exchanges before reaching the distal RCA. Lesion preparation used 2.0 mm and 1.5 mm NC balloons in the RCA. IVUS showed LAD diameters of 2.5mm distally with diffuse disease and < 40%plaque burden. A hybrid revascularization strategy was planned. Further preparation involved 3.0 mm and 2.0 mm balloons in the LAD and RCA. DCBs (2.0 ×25 mm in distal LAD; 2.0 × 20 mm in RCA) were applied for 60 seconds each. A Xience Sierra 3.0 × 38 mm DES was deployed in the proximal–mid LAD,post-dilated with 3.0–3.5 mm NC balloons and optimized with a 4.0 mm POT. IVUS revealed a distal edge dissection, covered with an additional overlapping Xience Sierra 2.75 × 23 mm DES. Final IVUS confirmed good stent expansion (MSA6 mm²), and angiography showed non–flow-limiting distal LAD dissection with TIMI 3 flow in both LAD and RCA.
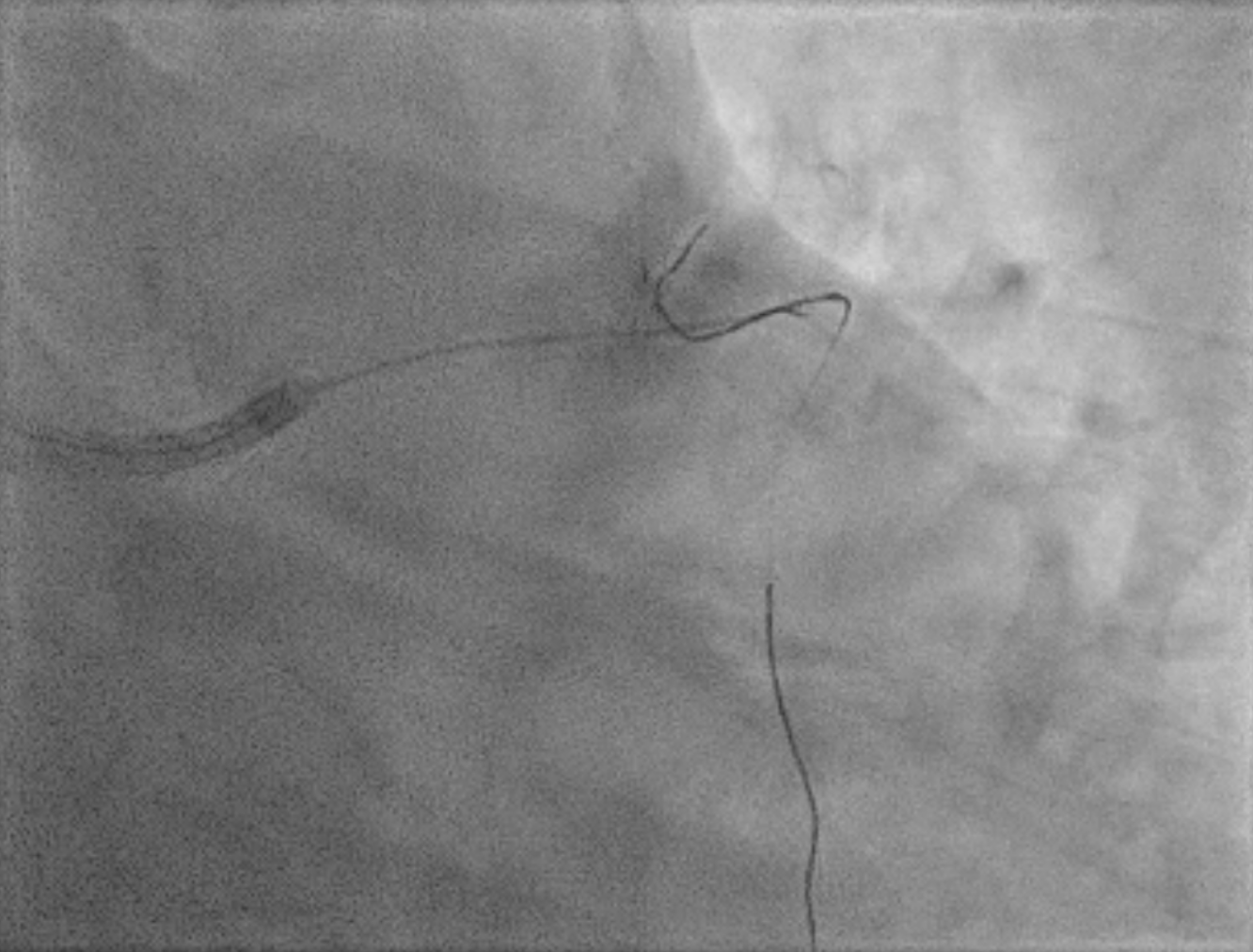
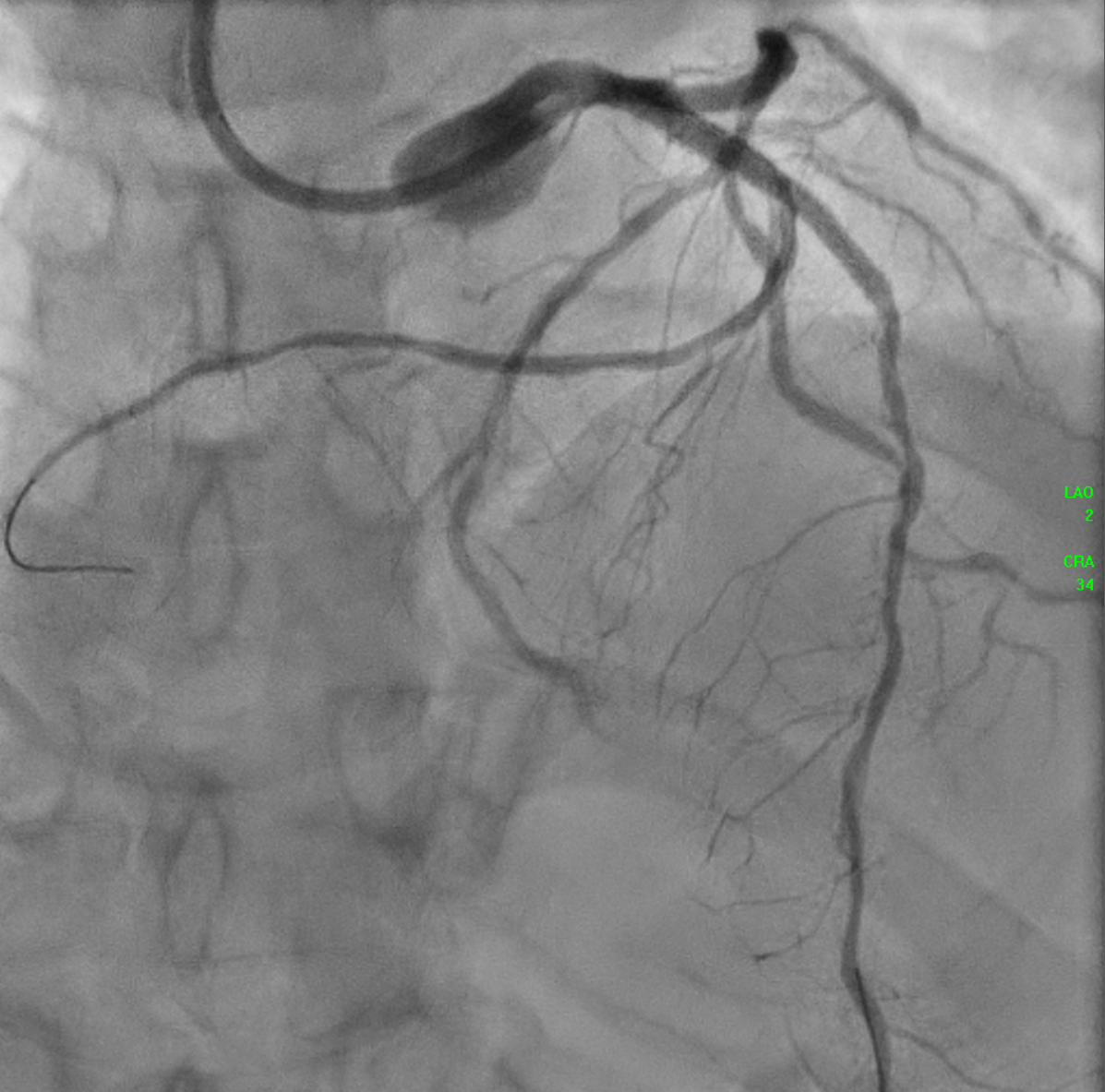
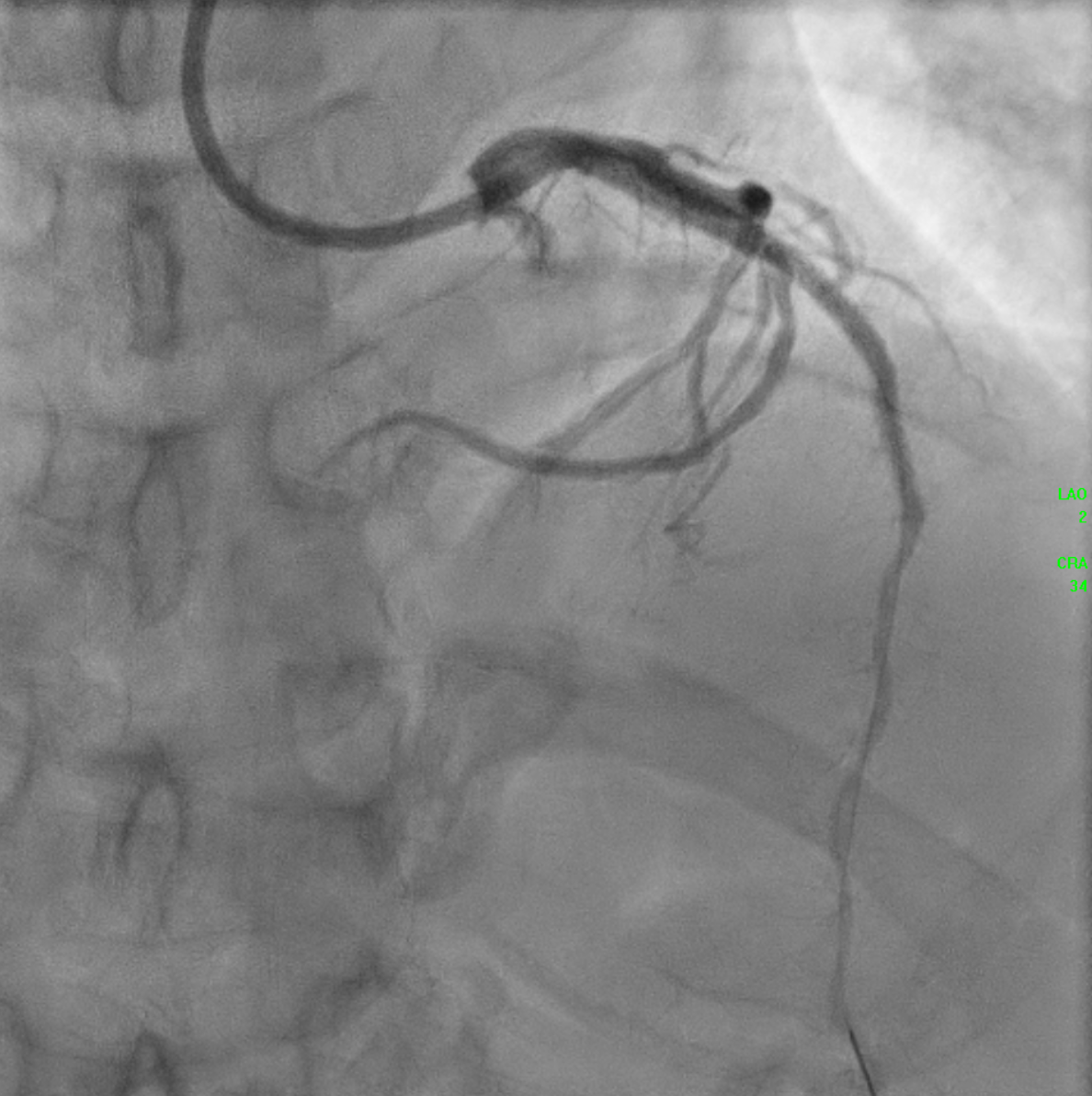
 3 wiring septal.mp4
3 wiring septal.mp4
 18 Angio post stent, distal stent edge dissection.mp4
18 Angio post stent, distal stent edge dissection.mp4
 21 Final Angio.mp4
21 Final Angio.mp4



Case Summary
In this rare case of a single coronary artery with the RCA arising from the LAD, a complex PCI was successfully performed using IVUS guidance and advanced wiring strategies. A hybrid approach with drug-eluting stents and drug-coated balloons achieved excellent final result. This case emphasizes that detailed imaging, careful technique selection, and readiness for anatomical challenges are key to success in high-risk anomalous coronary interventions.
