Lots of interesting abstracts and cases were submitted for TCTAP 2026. Below are the accepted ones after a thorough review by our official reviewers. Don’t miss the opportunity to expand your knowledge!
CASE20251106_019
Nightmare at Midnight: Troubleshooting in Left Main Stenting
By Hsuan-Ling Tseng
Presenter
Hsuan-Ling Tseng
Authors
Hsuan-Ling Tseng1
Affiliation
Chi-Mei Medical Center, Taiwan1
View Study Report
CASE20251106_019
Coronary - Complex PCI - Left Main
Nightmare at Midnight: Troubleshooting in Left Main Stenting
Hsuan-Ling Tseng1
Chi-Mei Medical Center, Taiwan1
Clinical Information
Relevant Clinical History and Physical Exam
A 60-year-old woman with CAD (2-V-D), s/p PCI with DES to mLAD and pLCX on 11/13/2024 (LM 40% stenosis), T2DM, hypertension, and dyslipidemia, presented with sudden chest tightness and dyspnea at midnight on 05/29/2025. Vital signs: T 37.4 °C, P 91/min, R 18/min, BP 162/84 mmHg. Appeared anxious but alert; lungs with bilateral basal rales; heart sounds regular, no murmur.

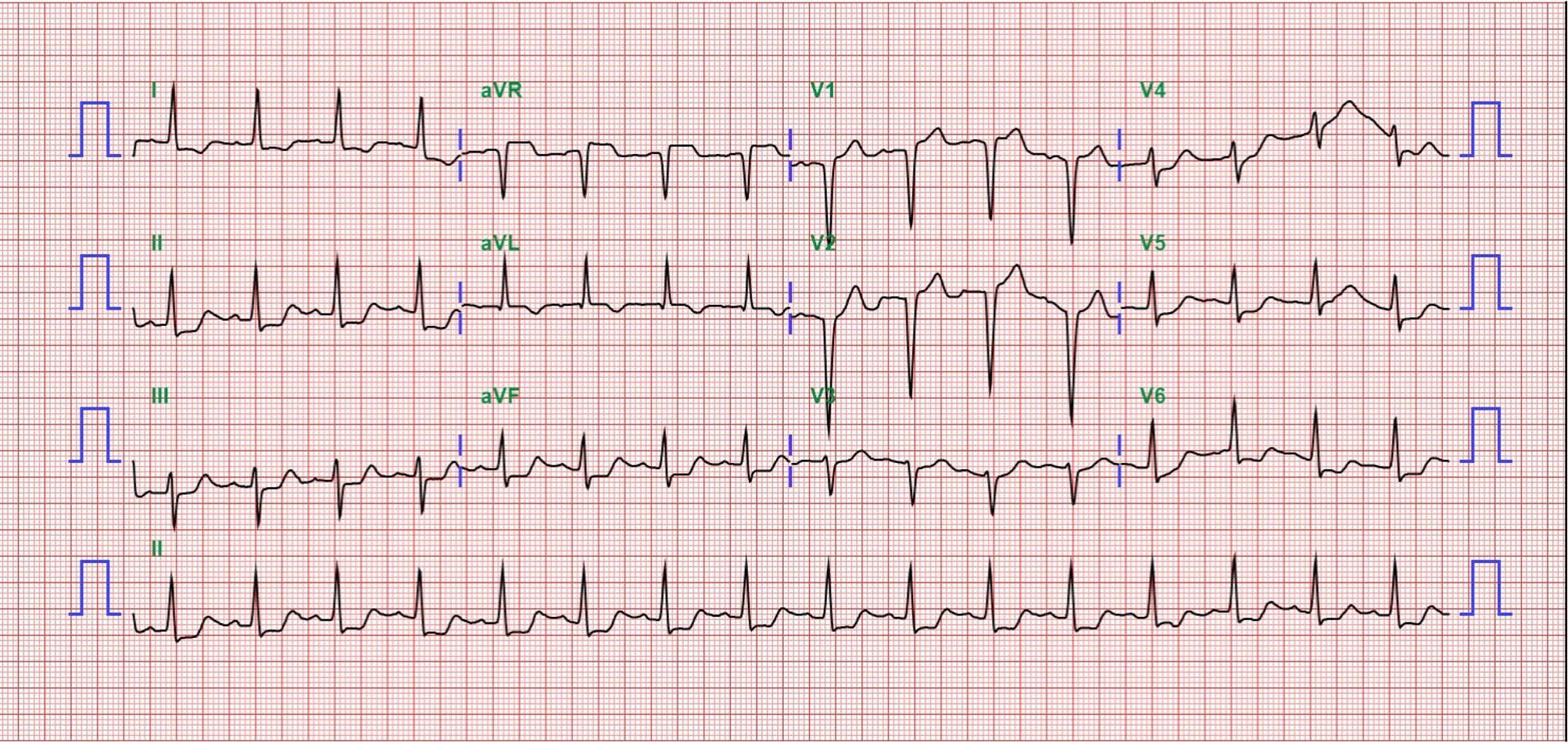
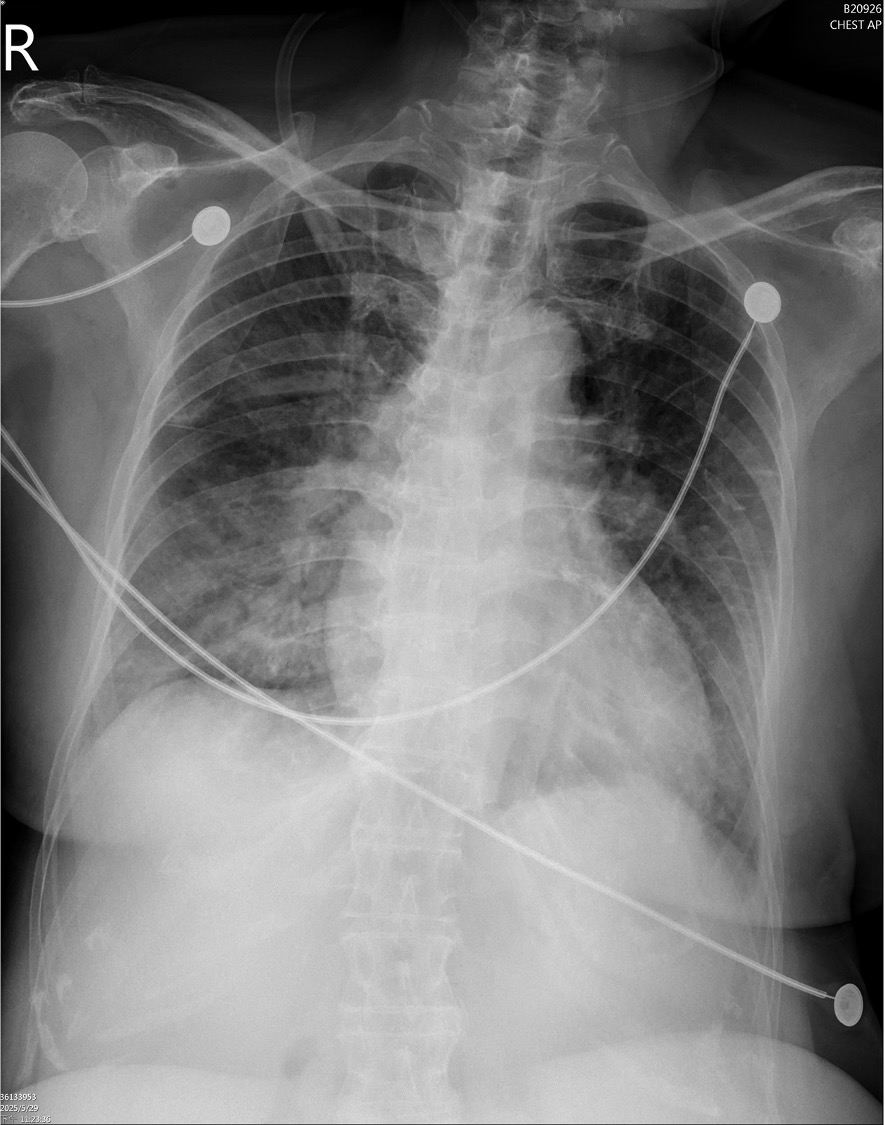
Relevant Test Results Prior to Catheterization
ECG showed ST elevation in aVR with diffuse ST depression. Chest X-ray revealed bilateral pulmonary edema. Laboratory data demonstrated elevated hs-troponin I (1012 pg/mL). Bedside TTE revealed global hypokinesis with an estimated LVEF of 40%.
 A4C.mp4
A4C.mp4
 LAX.mp4
LAX.mp4


Relevant Catheterization Findings
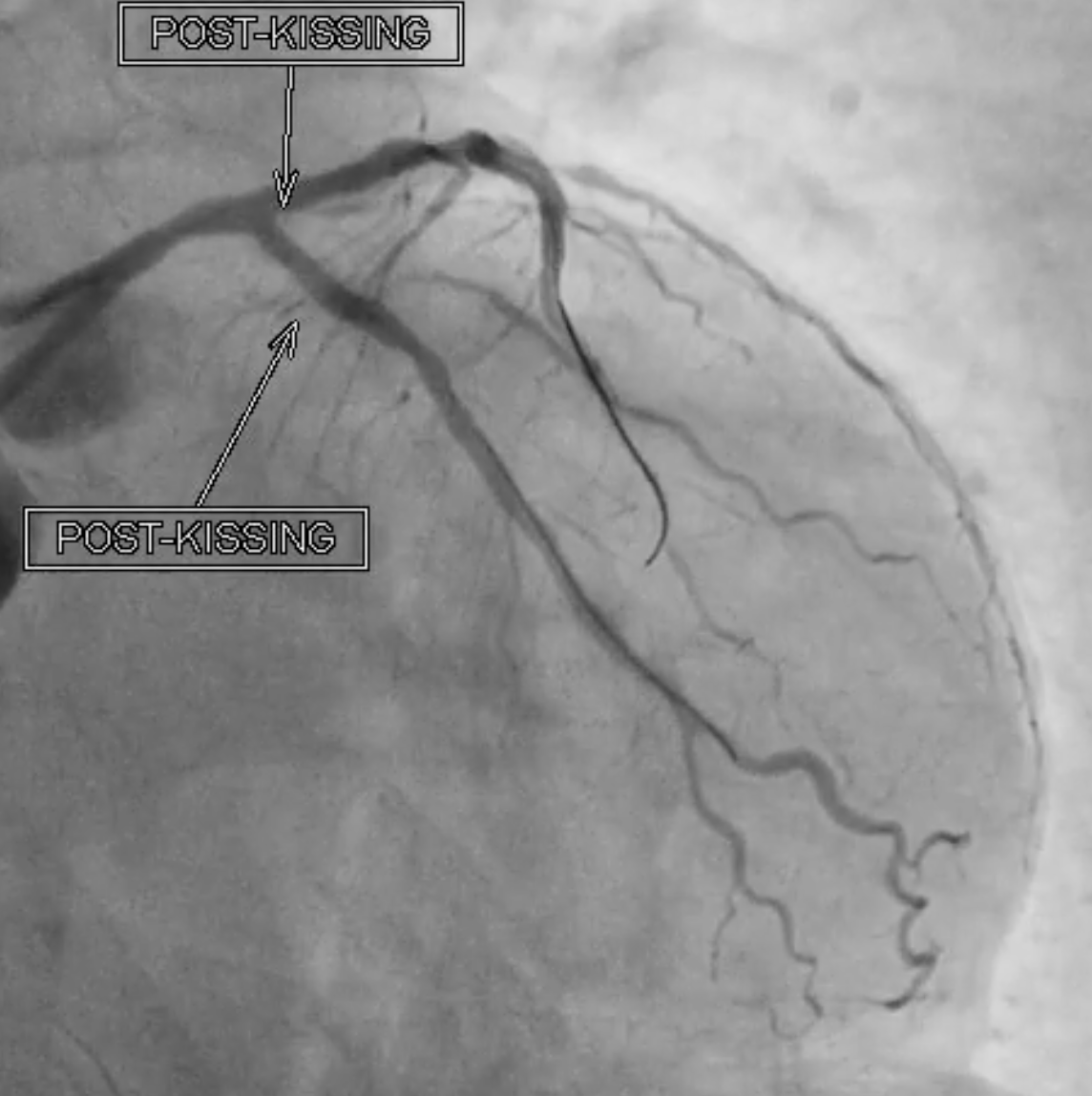
Severe CAD with LM + 3-vessel disease. dLM and shaft: critical stenosis; pLAD: critical stenosis; mLAD: s/p DES with stent underexpansion and proximal stent-edge restenosis; pLCX: s/p DES with proximal stent-edge restenosis; mRCA: 50% stenosis. SYNTAX score: 44.
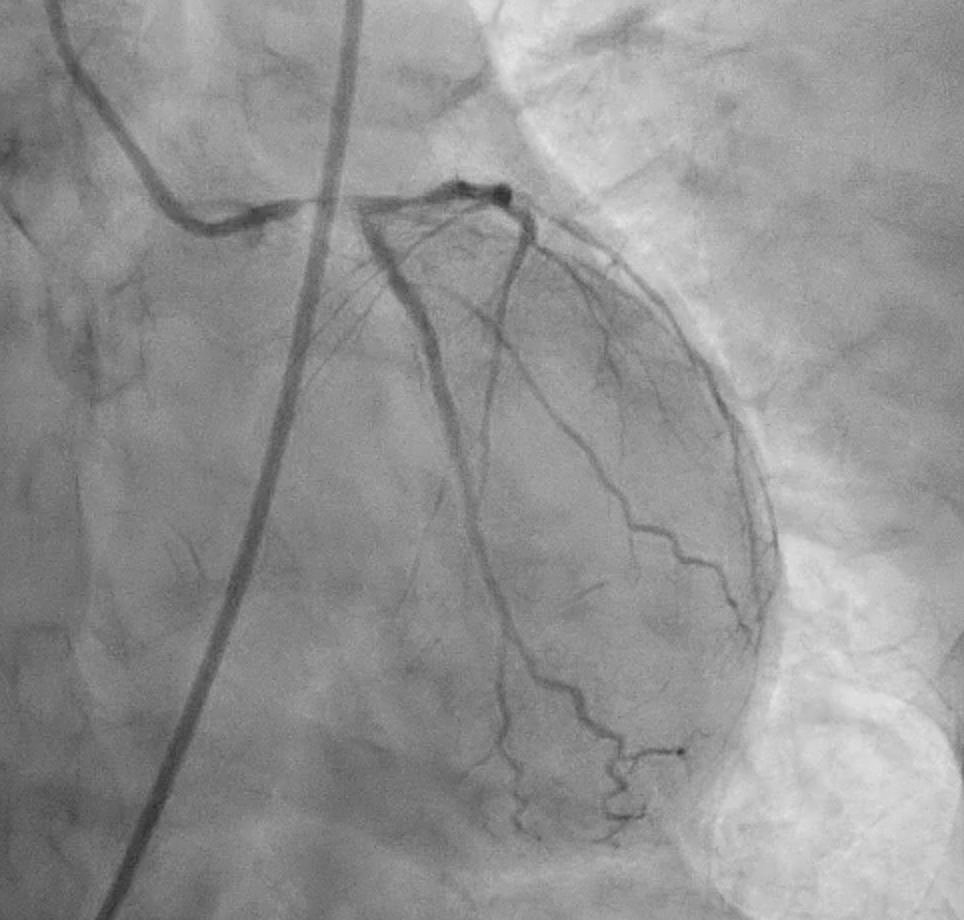
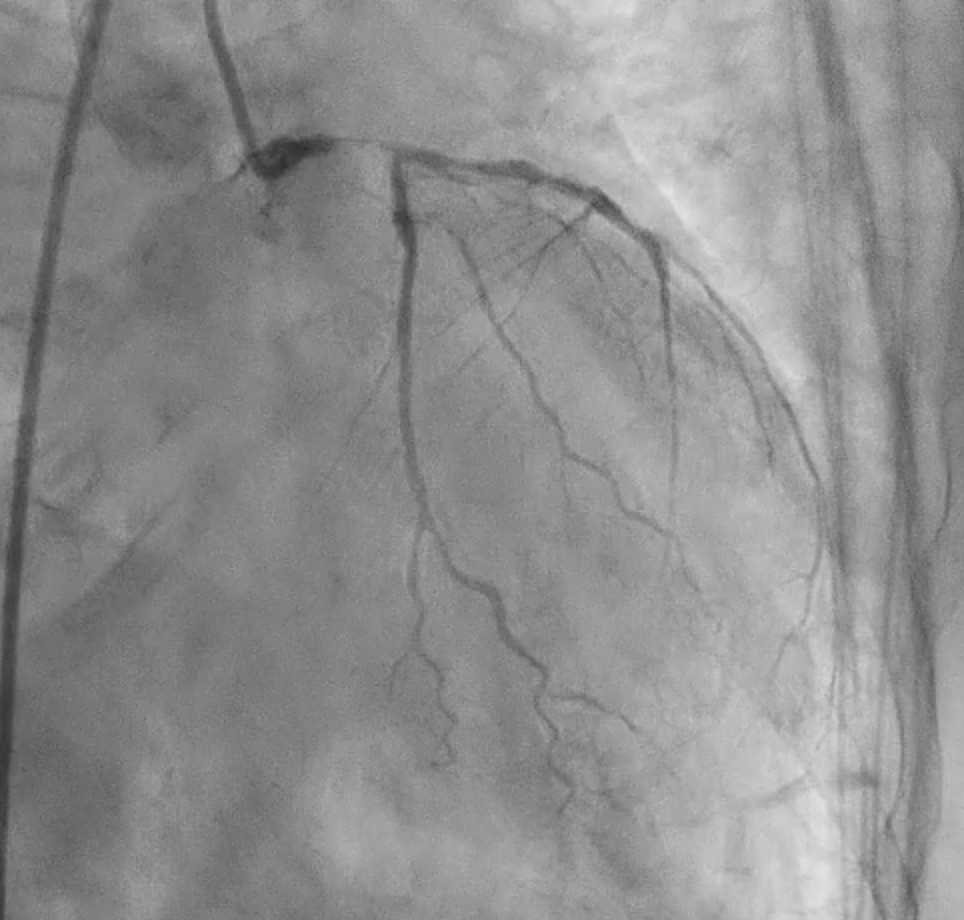
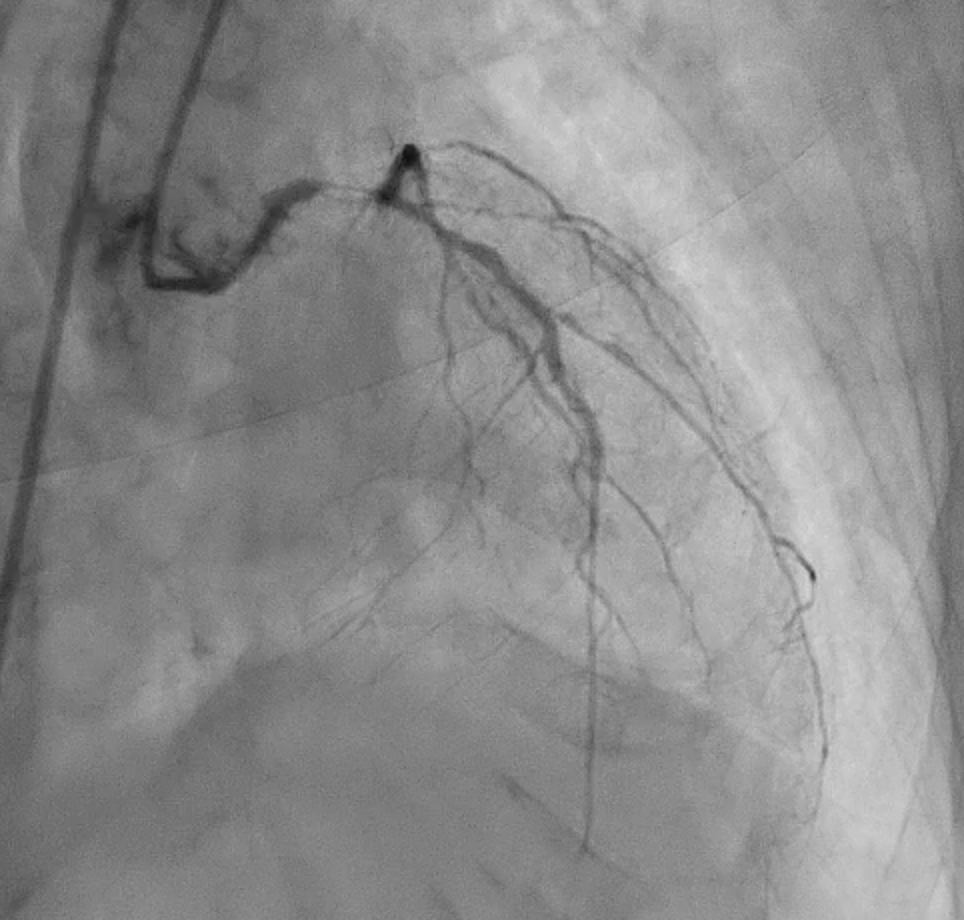
 CAG(6).mp4
CAG(6).mp4
 CAG(8).mp4
CAG(8).mp4
 CAG(10).mp4
CAG(10).mp4



Interventional Management
Procedural Step
Under IABP (left femoral), PCI via right brachial with 6 Fr EBU 3.5. Runthrough to LAD, Sion Blue to LCX. Predilation of LM/pLAD with 2.0×20 mm balloon; IVUS pullbacks. Further dilatation with 2.5×20 mm NC for mLAD underexpansion, pLAD, and LM. oLCX de novo and pLCX edge ISR predilated with 2.5×20 mm NC; LCX ISR treated with DCB 2.5×20 mm. Szabo technique attempted for LM–LAD with a 3.0×24 mm DES; the undeployed stent dislodged during repositioning and was deployed at the dislodgement site. IVUS showed 2–3 struts protruding into the aorta from the LM ostium and incomplete pLAD coverage. Post-dilation with 3.5×20 and 2.5×20 mm NC; DCB 3.0×20 mm for pLAD uncovered plaque and mLAD proximal edge ISR. Final CAG: TIMI 3 flow.At 3 months, staged PCI via right radial with 6 Fr EBU 3.5. Sion Blue ES to distal LAD. IVUS: mLAD stent underexpansion (MSA <2.0 mm²); wire not through struts. IVL 3.5×12 mm initially could not cross LM; after guide exchange (JL 3.5, then EBU 3.0/3.5), IVL advanced to mLAD and delivered 100 shocks, producing a ring crack and area gain. Further dilation with 3.0×20 and 3.5×20 mm NC. IVUS: pLAD type B dissection without flow limitation. DCB 3.5×40 mm to p–mLAD. LM ostial stent further dilated with 3.5×20 mm. Final CAG: TIMI 3 flow.
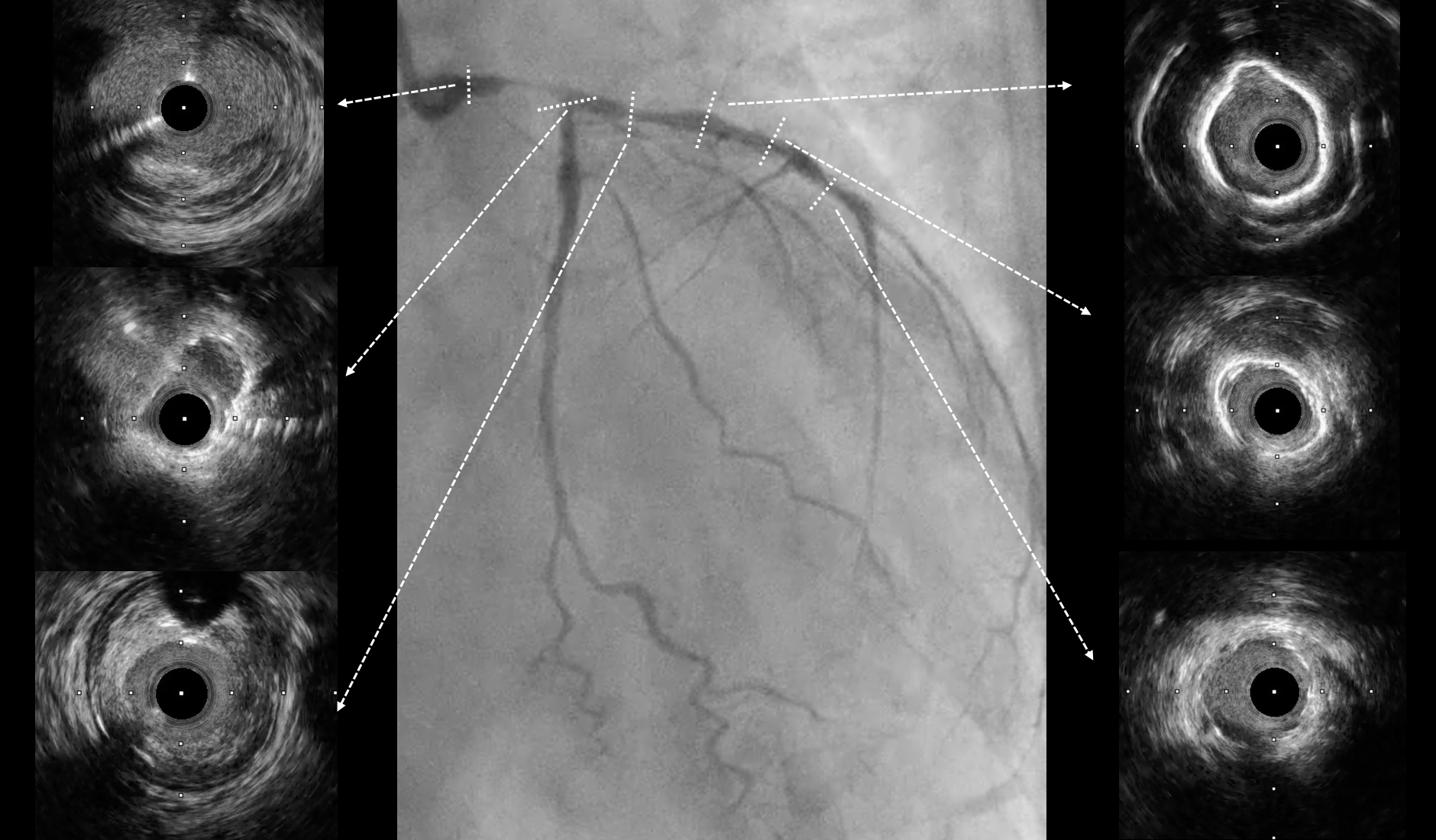
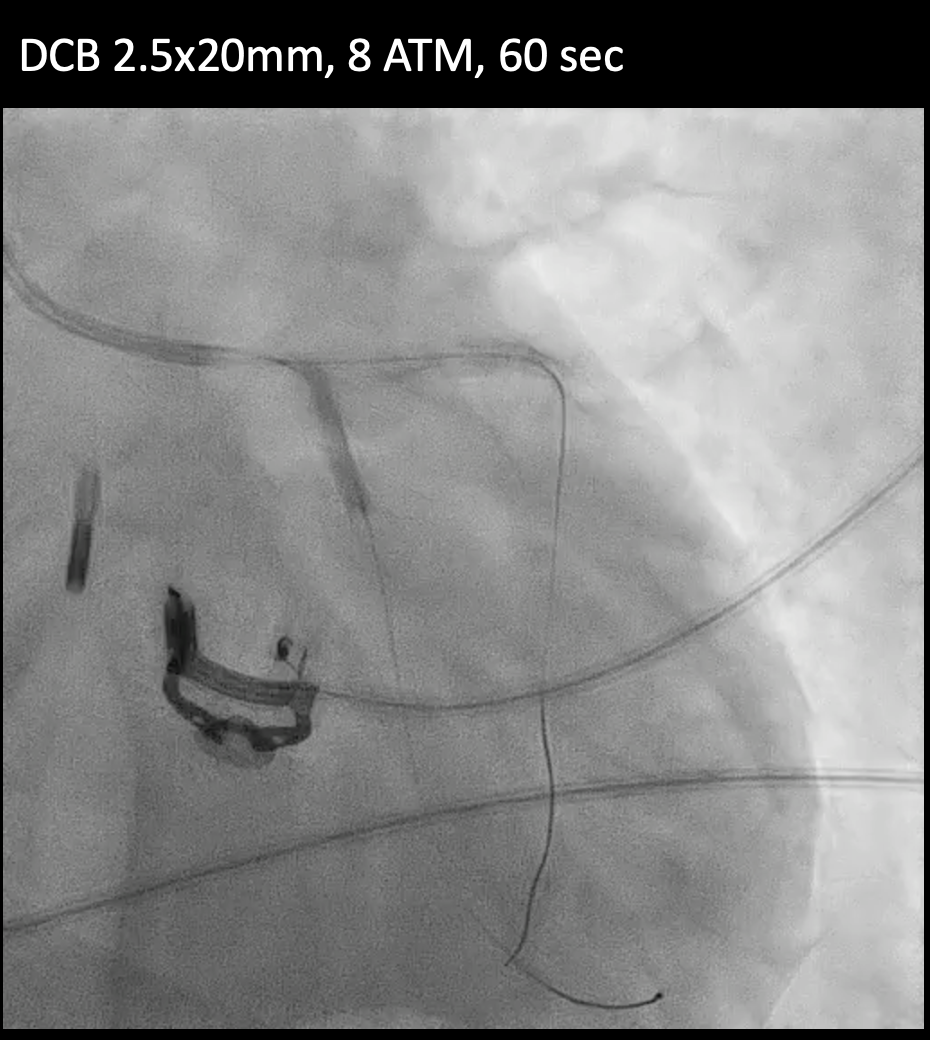
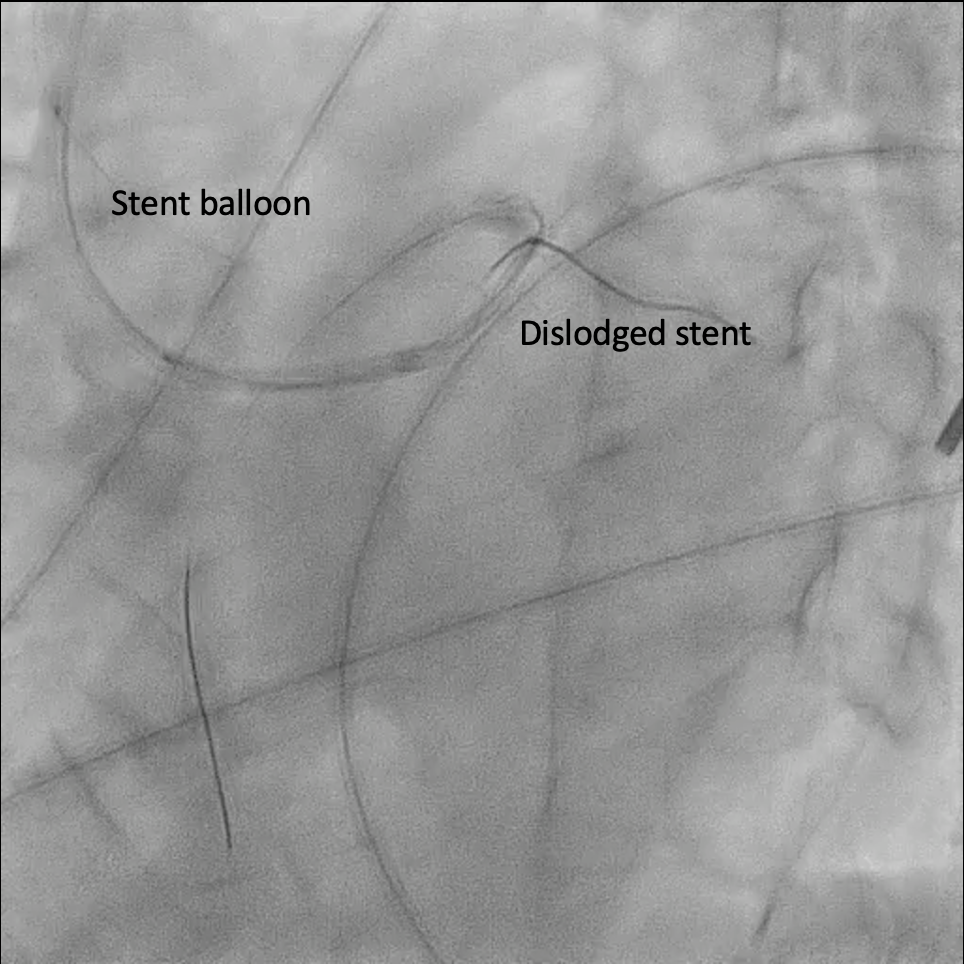
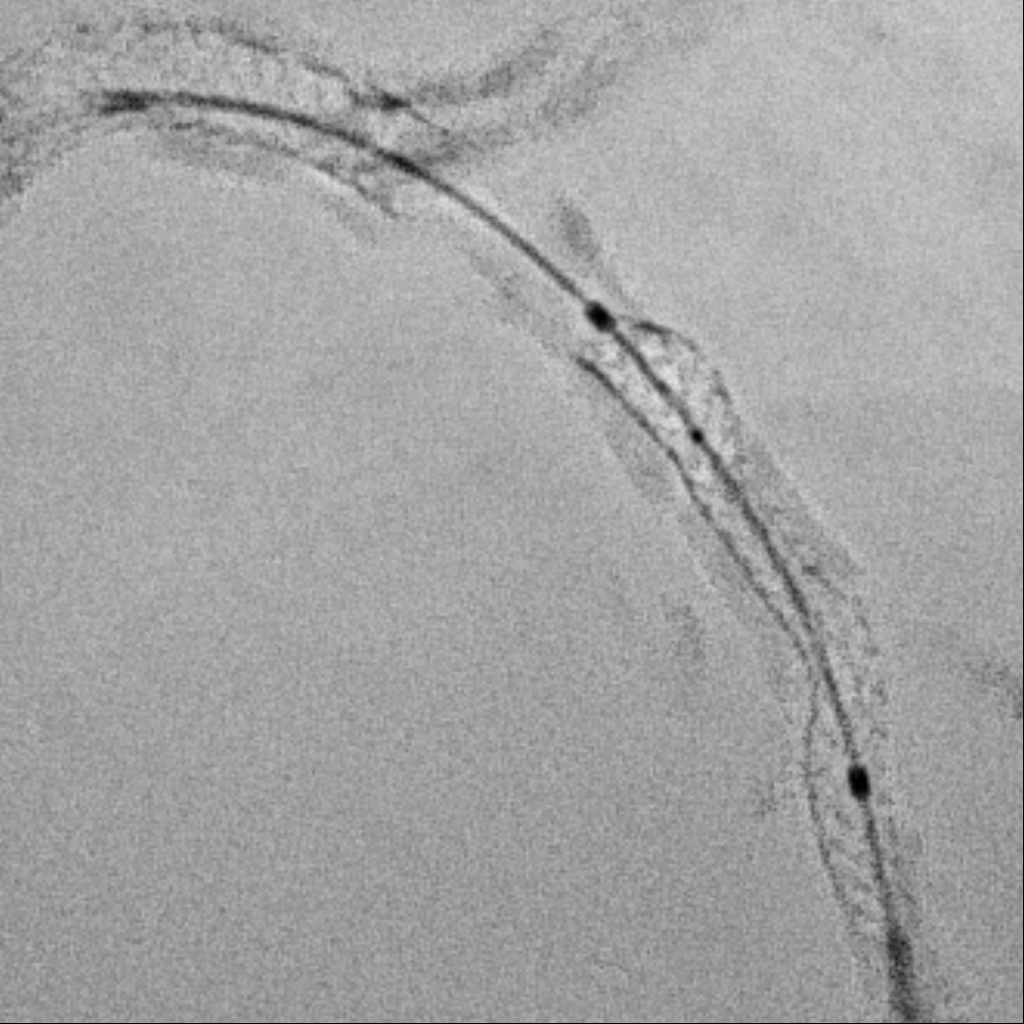
 CAG(38).mp4
CAG(38).mp4
 CAG(61).mp4
CAG(61).mp4
 IVL(61).mp4
IVL(61).mp4




Case Summary
Timing matters as much as technique—operator fatigue and suboptimal midnight conditions can silently amplify risks in complex PCI. Past success can bias current judgment; repeating a previously effective technique may overlook new anatomical nuances. Guiding catheter engagement is double-edged: while it enhances support, it compromises precision at the ostium. Preparation should anticipate rare complications, not just manage common ones.
