Lots of interesting abstracts and cases were submitted for TCTAP 2026. Below are the accepted ones after a thorough review by our official reviewers. Don’t miss the opportunity to expand your knowledge!
ABS20251114_0016
Intravascular Imaging Guidance for Percutaneous Coronary Intervention in Diabetes and Long Diffuse Coronary Lesions: A Large Meta-Analysis
By Hendrianus Hendrianus, Sang Yeub Lee, Hoyoun Won, Wang-Soo Lee, Young-Hoon Jeong, Jun Hwan Cho, Woo Jin Jang, Sang-Wook Kim
Presenter
Hendrianus Hendrianus
Authors
Hendrianus Hendrianus1, Sang Yeub Lee1, Hoyoun Won2, Wang-Soo Lee2, Young-Hoon Jeong1, Jun Hwan Cho1, Woo Jin Jang2, Sang-Wook Kim1
Affiliation
Heart and Brain Hospital, Chung-Ang University Medical Center, Korea (Republic of)1, Chung-Ang University Hospital, Korea (Republic of)2
View Study Report
ABS20251114_0016
Invasive Imaging (IVUS, OCT, NIRS, VH, etc)
Intravascular Imaging Guidance for Percutaneous Coronary Intervention in Diabetes and Long Diffuse Coronary Lesions: A Large Meta-Analysis
Hendrianus Hendrianus1, Sang Yeub Lee1, Hoyoun Won2, Wang-Soo Lee2, Young-Hoon Jeong1, Jun Hwan Cho1, Woo Jin Jang2, Sang-Wook Kim1
Heart and Brain Hospital, Chung-Ang University Medical Center, Korea (Republic of)1, Chung-Ang University Hospital, Korea (Republic of)2
Background
While intravascular imaging (IVUS/OCT) improves outcomes in percutaneous coronary intervention (PCI), its benefit profile across diabetes status and lesion length remains incompletely defined.
Methods
We systematically searched PubMed, Embase, and CENTRAL for randomized controlled trials (RCTs) comparing intravascular imaging- versus angiography-guided PCI, or OCT versus IVUS, that reported outcomes stratified by diabetes status or lesion characteristics. The primary efficacy outcome was target vessel failure (TVF) at ≥1-year follow-up. Data were analyzed using random-effects models.
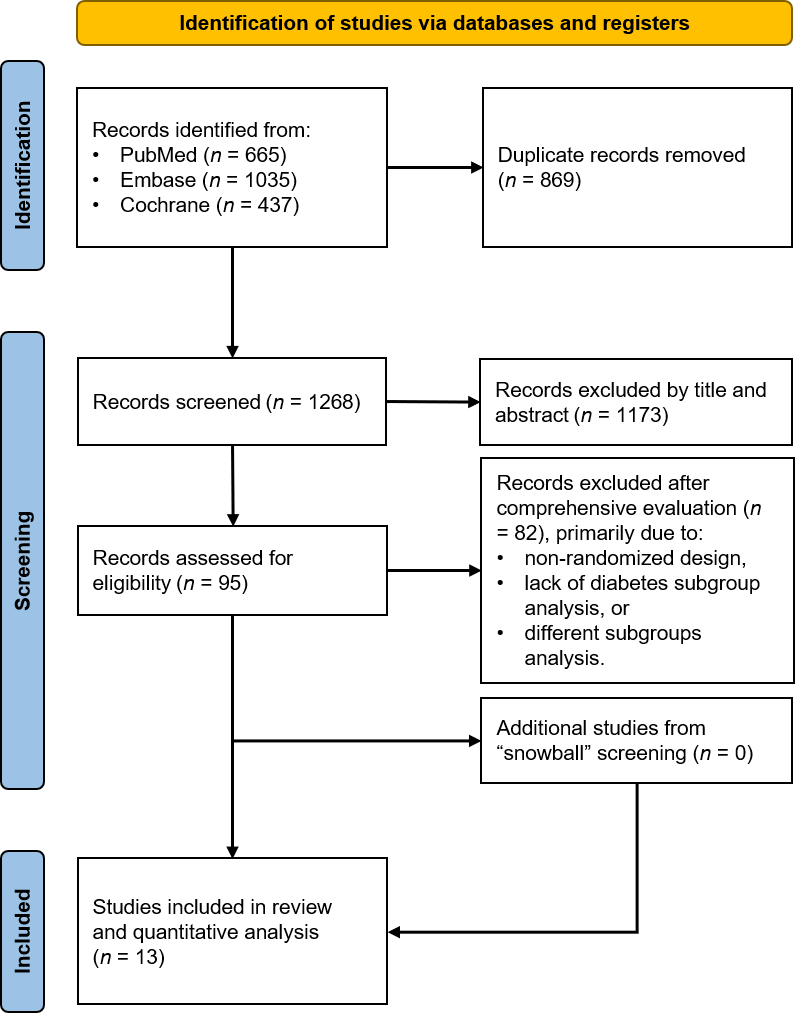

Results
Thirteen RCTs (n=18,379) were included. Intravascular imaging significantly reduced TVF by 33% compared to angiography (RR 0.67, 95% CI 0.58-0.78; p<0.001), with consistent benefits in both patients with diabetes (RR 0.69, 95% CI 0.53-0.90; p=0.006) and without diabetes (RR 0.65, 95% CI 0.55-0.77; p<0.001; p-interaction=0.72). The treatment benefit was consistent across complex PCI populations and with both IVUS and OCT guidance. In diabetic patients undergoing complex PCI (RR 0.74, 95% CI 0.53-1.04) or receiving OCT guidance (RR 0.70, 95% CI 0.42-1.16), point estimates favored intravascular imaging but did not reach statistical significance. In direct head-to-head comparison, OCT demonstrated similar TVF risk to IVUS (RR 1.01, 95% CI 0.65-1.55; p=0.97), with consistent results across diabetes status. Analysis by lesion length revealed substantial benefit in long lesions (RR 0.66, 95% CI 0.55-0.80; p<0.0001) compared to short lesions (RR 0.88, 95% CI 0.66-1.19; p=0.41; p-interaction=0.11). Meta-regression analysis identifies age and follow-up duration as significant effect modifiers for TVF in diabetes.
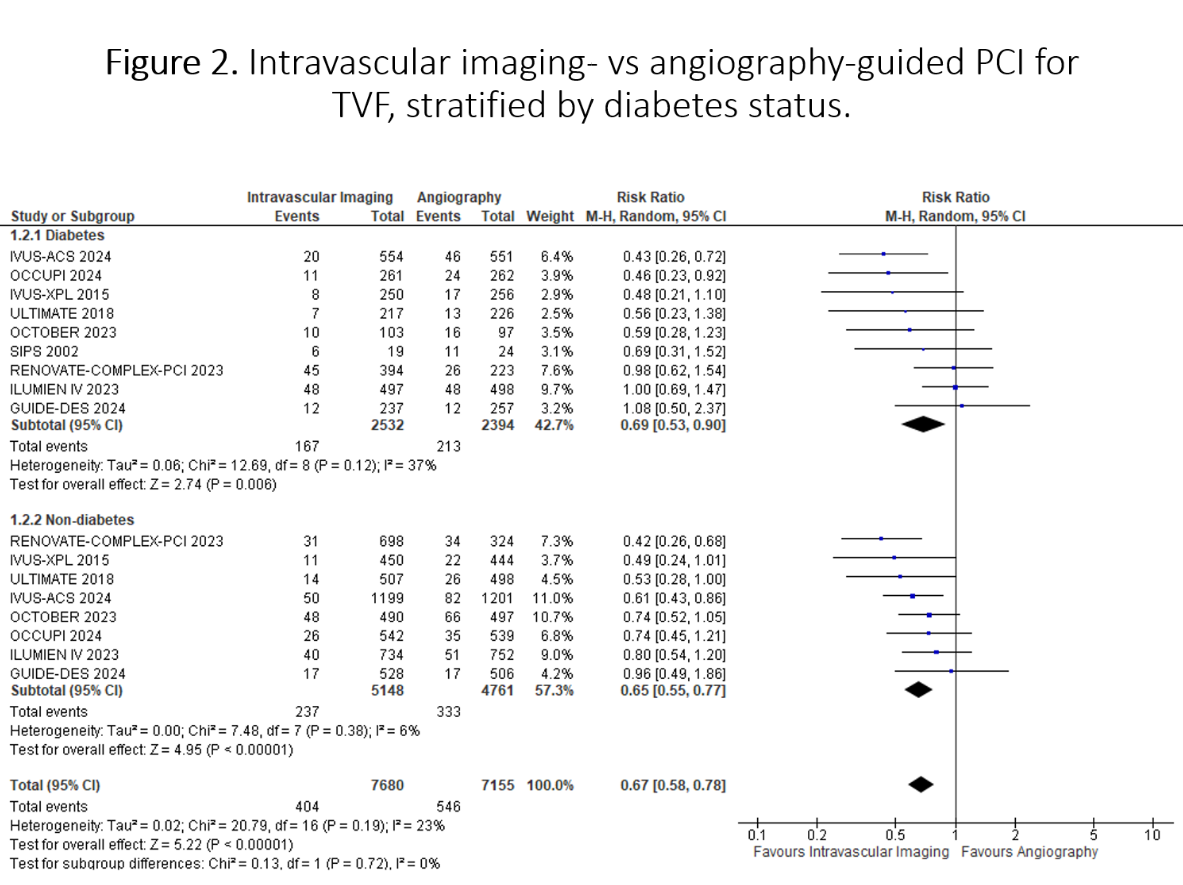
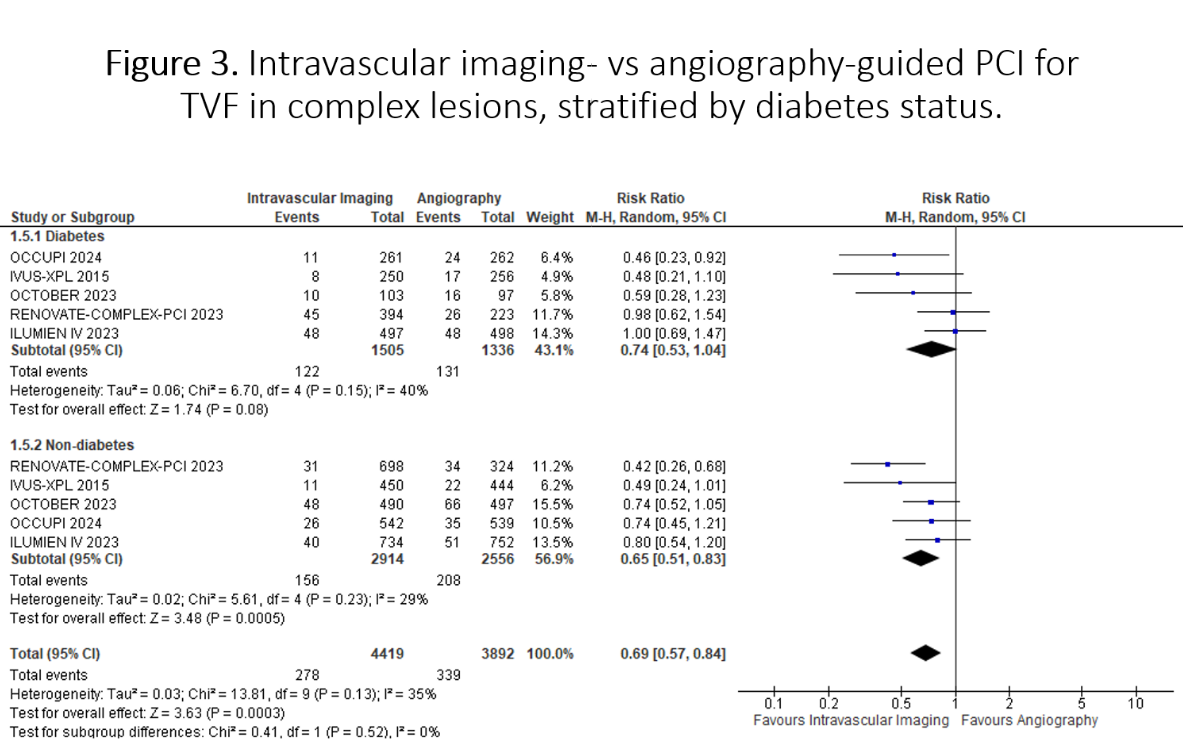
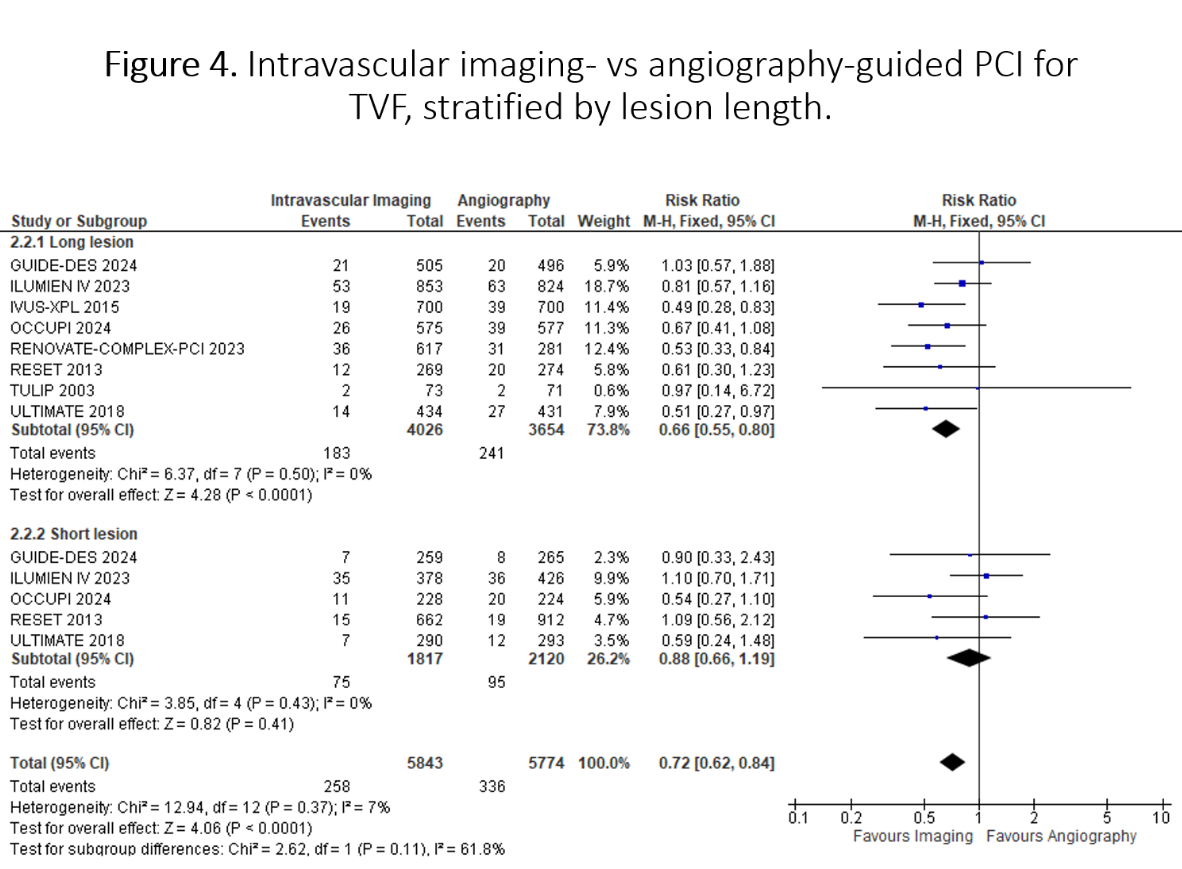



Conclusion
This novel meta-analysis of RCTs demonstrates that intravascular imaging-guided PCI significantly reduces TVF, with consistent benefits across diabetes status. The treatment effect is particularly pronounced in long lesions, while OCT and IVUS show comparable efficacy. These findings support broader implementation of intravascular imaging, especially in patients with diabetes and those with long coronary lesions.
