Lots of interesting abstracts and cases were submitted for TCTAP 2026. Below are the accepted ones after a thorough review by our official reviewers. Don’t miss the opportunity to expand your knowledge!
ABS20251107_0021
Complete Revascularization in Multivessel STEMI and Prognostic Comparison With Single Vessel Disease: Insights From the Mie ACS Registry
By Akihiro Takasaki
Presenter
Akihiro Takasaki
Authors
Akihiro Takasaki1
Affiliation
Mie University Hospital, Japan1
View Study Report
ABS20251107_0021
ACS/AMI
Complete Revascularization in Multivessel STEMI and Prognostic Comparison With Single Vessel Disease: Insights From the Mie ACS Registry
Akihiro Takasaki1
Mie University Hospital, Japan1
Background
The prognostic benefit of complete revascularization (CR) in multivessel disease (MVD) with ST-segment elevation myocardial infarction (STEMI) is established, yet whether outcomes after CR in MVD approximate those of single-vessel disease (SVD) remains uncertain.
Methods
We analyzed 3,980 STEMI patients undergoing primary PCI between 2013 and 2022 from the Mie ACS Registry. Patients with cardiogenic shock, prior CABG, non-culprit chronic total occlusion, or surgical indication were excluded. Subjects were categorized as SVD (n=2,347), MVD+CR (n=381), or MVD+non-CR (n=1,252). The primary outcome was 2-year major adverse cardiovascular events (MACE), defined as cardiovascular death, nonfatal myocardial infarction, hospitalization for heart failure, or unstable angina.
Results
Kaplan–Meier analysis demonstrated significantly higher MACE in the MVD+non-CR group compared with both SVD and MVD+CR (log-rank P<0.001). In contrast, outcomes between SVD and MVD+CR were comparable, with no significant difference in all-cause death (P=0.332), cardiovascular death (P=0.584), or MACE (P=0.943). These findings were consistent in propensity score–matched analyses.
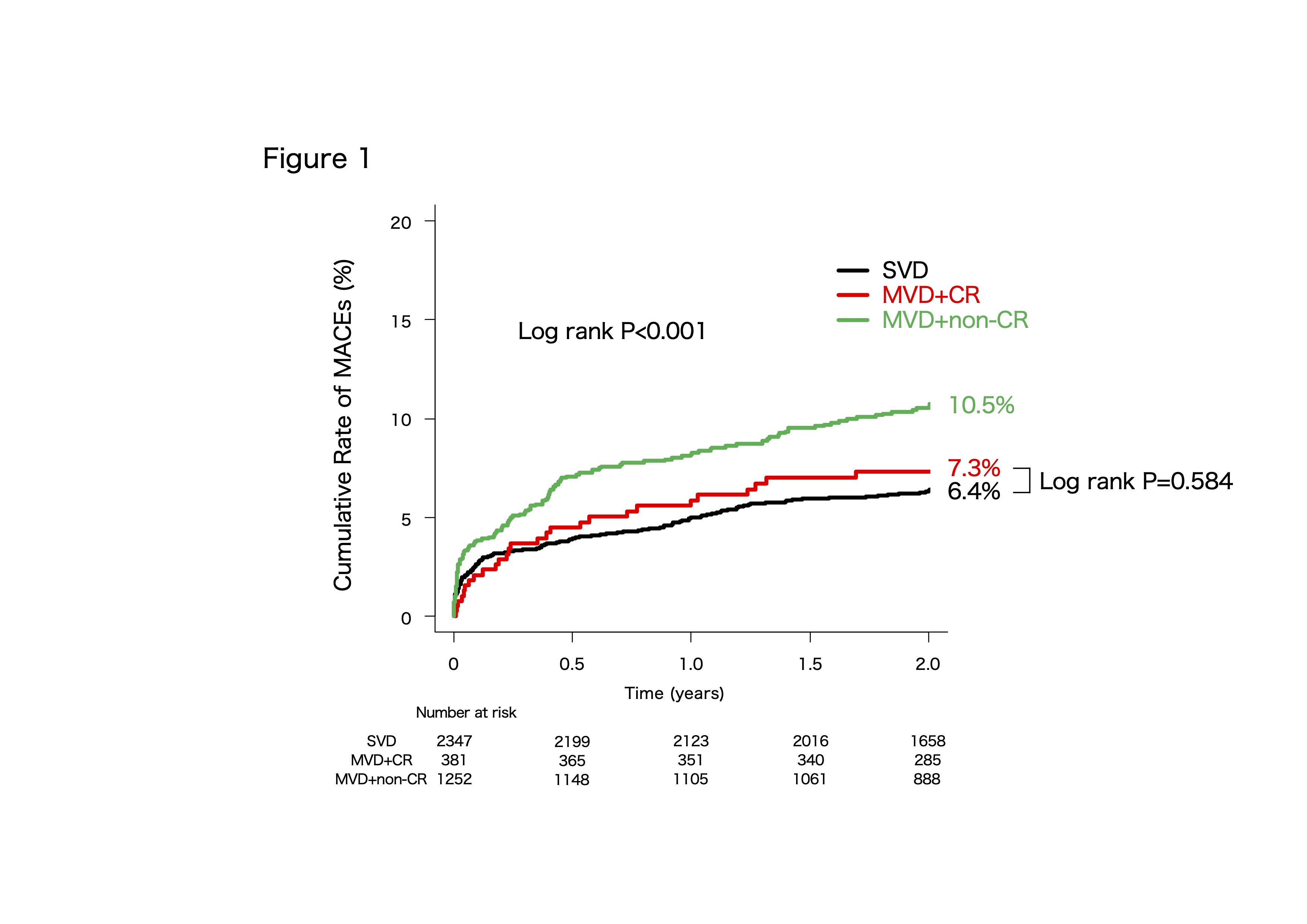

Conclusion
In this real-world registry, STEMI patients with MVD who achieved complete revascularization had 2-year outcomes comparable to those with SVD, whereas incomplete revascularization was associated with worse prognosis. These results underscore the prognostic importance of pursuing CR in suitable MVD patients.
