Lots of interesting abstracts and cases were submitted for TCTAP 2026. Below are the accepted ones after a thorough review by our official reviewers. Don’t miss the opportunity to expand your knowledge!
ABS20251107_0008
Efficacy and Clinical Outcomes of IVUS vs. Angiography-Guided PCI (Superior Benefit in Complex Lesions but Not in Simple PCI): Systematic Review and Meta-Analysis
By Lutfi Hafiz Zunardi
Presenter
Lutfi Hafiz Zunardi
Authors
Lutfi Hafiz Zunardi1
Affiliation
Sunan Kalijaga General Hospital, Indonesia1
View Study Report
ABS20251107_0008
Invasive Imaging (IVUS, OCT, NIRS, VH, etc)
Efficacy and Clinical Outcomes of IVUS vs. Angiography-Guided PCI (Superior Benefit in Complex Lesions but Not in Simple PCI): Systematic Review and Meta-Analysis
Lutfi Hafiz Zunardi1
Sunan Kalijaga General Hospital, Indonesia1
Background
Intravascularultrasound (IVUS) can reduce angiographic ambiguity in patients undergoingpercutaneous coronary intervention (PCI). Although numerous studies havedemonstrated that intravascular imaging is valuable for guiding PCI, itsadoption remains limited due to high costs, particularly in developingcountries. This study aims to evaluate the clinical outcomes of PCI guided byintravascular imaging compared with those guided by angiography.
Methods
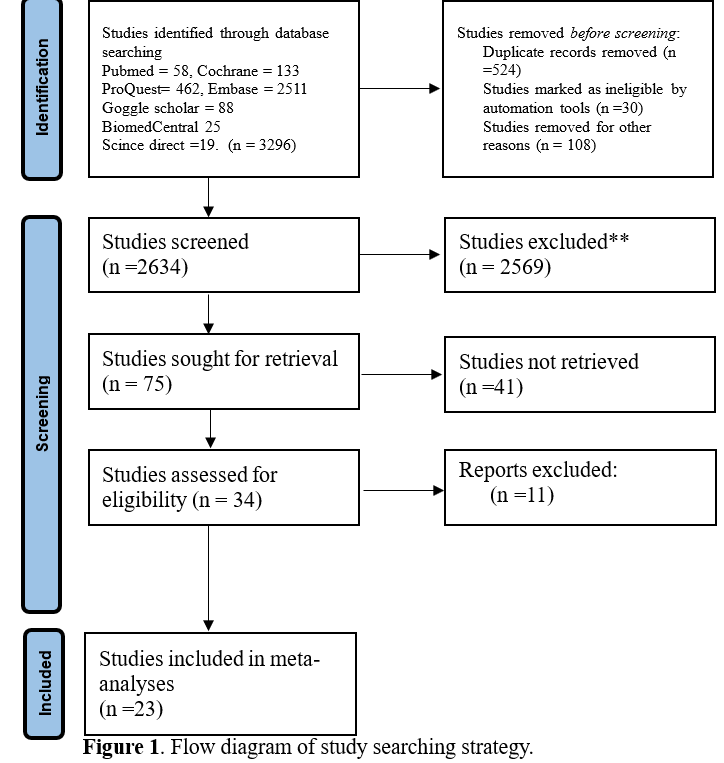
This research followed the PRISMA 2020 guidelines to ensure a systematic and transparent review process. A thorough search of the literature was conducted across major electronic databases PubMed, Embase, Web of Science, and the Cochrane Library, covering publications up to June 2025. The methodological quality of all eligible studies was evaluated using the Cochrane Risk of Bias Tool. Statistical analyses and data synthesis were subsequently performed using R software (version 4.1.3) and RevMan (version 5.3).

Results
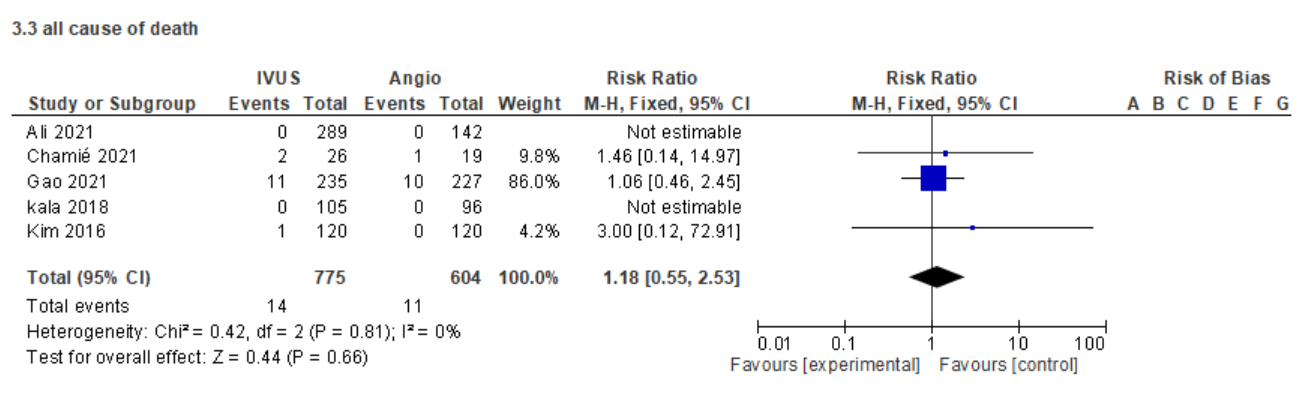
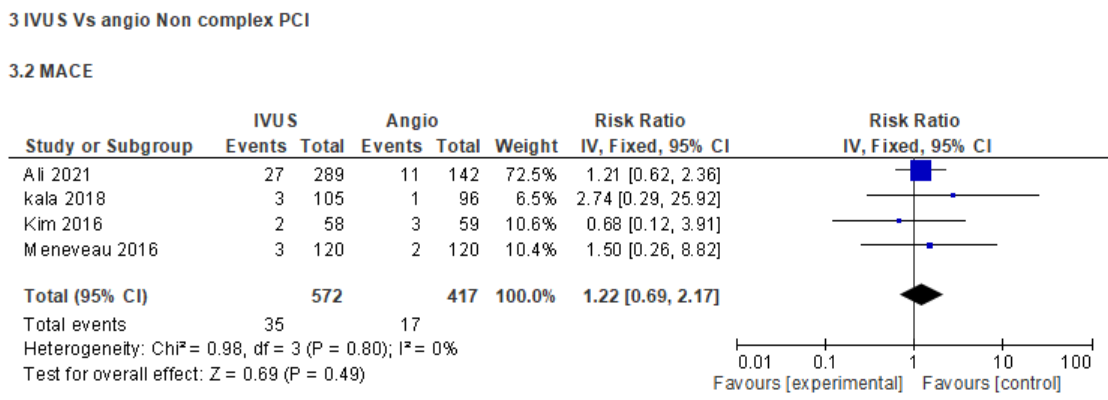
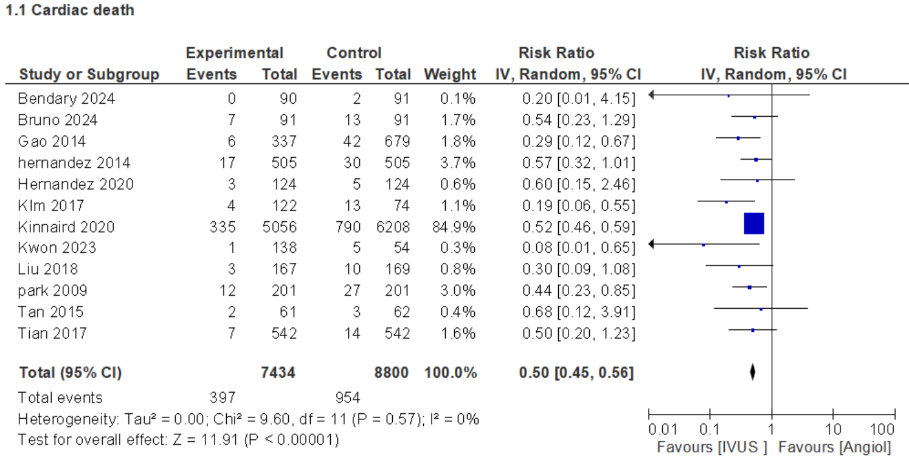
This meta-analysis included evidence from 23 studies, comprising both randomized and non-randomized controlled trials, with a total of 17,929 participants. Compared with angiography-guided PCI, intravascular imaging guidance was significantly associated with improved clinical outcomes and reduced adverse events. Specifically, major adverse cardiovascular events occurred in 6.2% versus 9.9%of patients (risk ratio [RR] 0.58; 95% confidence interval [CI] 0.50–0.67),cardiac death in 5.3% versus 10.8% (RR 0.50; 95% CI 0.45–0.56), and all-cause mortality in 7.4% versus 13.4% (RR 0.58; 95% CI 0.48–0.69). Myocardial infarction was observed in 2.7% versus 3.9% (RR 0.70; 95% CI 0.59–0.82),overall revascularization in 10% versus 17.1% (RR 0.61; 95% CI 0.44–0.85), stent thrombosis in 0.7% versus 2.5% (RR 0.30; 95% CI 0.16–0.54), target vessel revascularization in 7.2% versus 12.5% (RR 0.56; 95% CI 0.45–0.70), and target lesion revascularization in 4.9% versus 8.8% (RR 0.46; 95% CI 0.27–0.78).
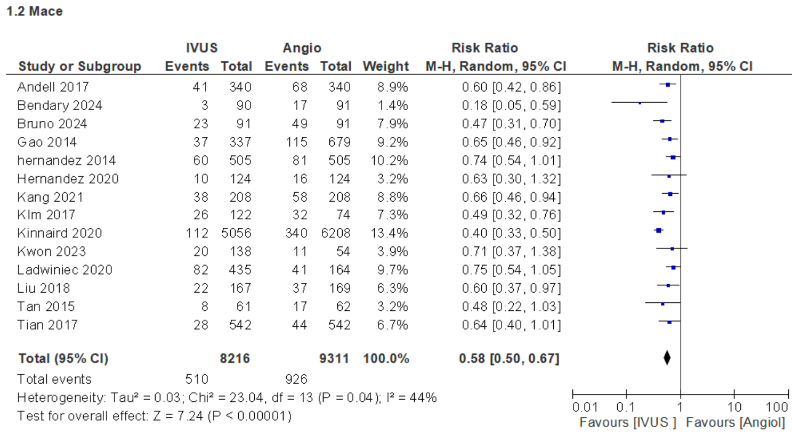
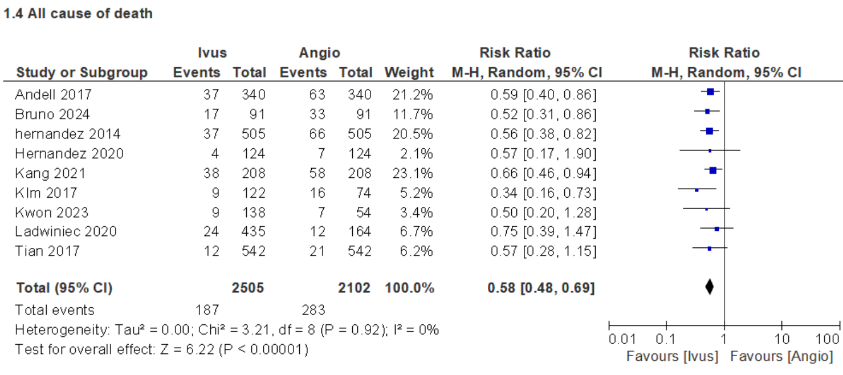



Conclusion
This meta-analysis demonstrates that IVUS-guided PCI significantly improves clinical outcomes and reduces major adverse cardiac events, mortality, and revascularization rates in patients with complex or left main coronary artery(LMCA) lesions. Nonetheless, in simple or non-complex PCI cases, IVUS guidance does not appear to provide a significant clinical benefit compared with angiography alone, suggesting that its routine use may be unnecessary in less complex interventions, particularly in resource-limited settings.