Lots of interesting abstracts and cases were submitted for TCTAP 2026. Below are the accepted ones after a thorough review by our official reviewers. Don’t miss the opportunity to expand your knowledge!
ABS20251102_0001
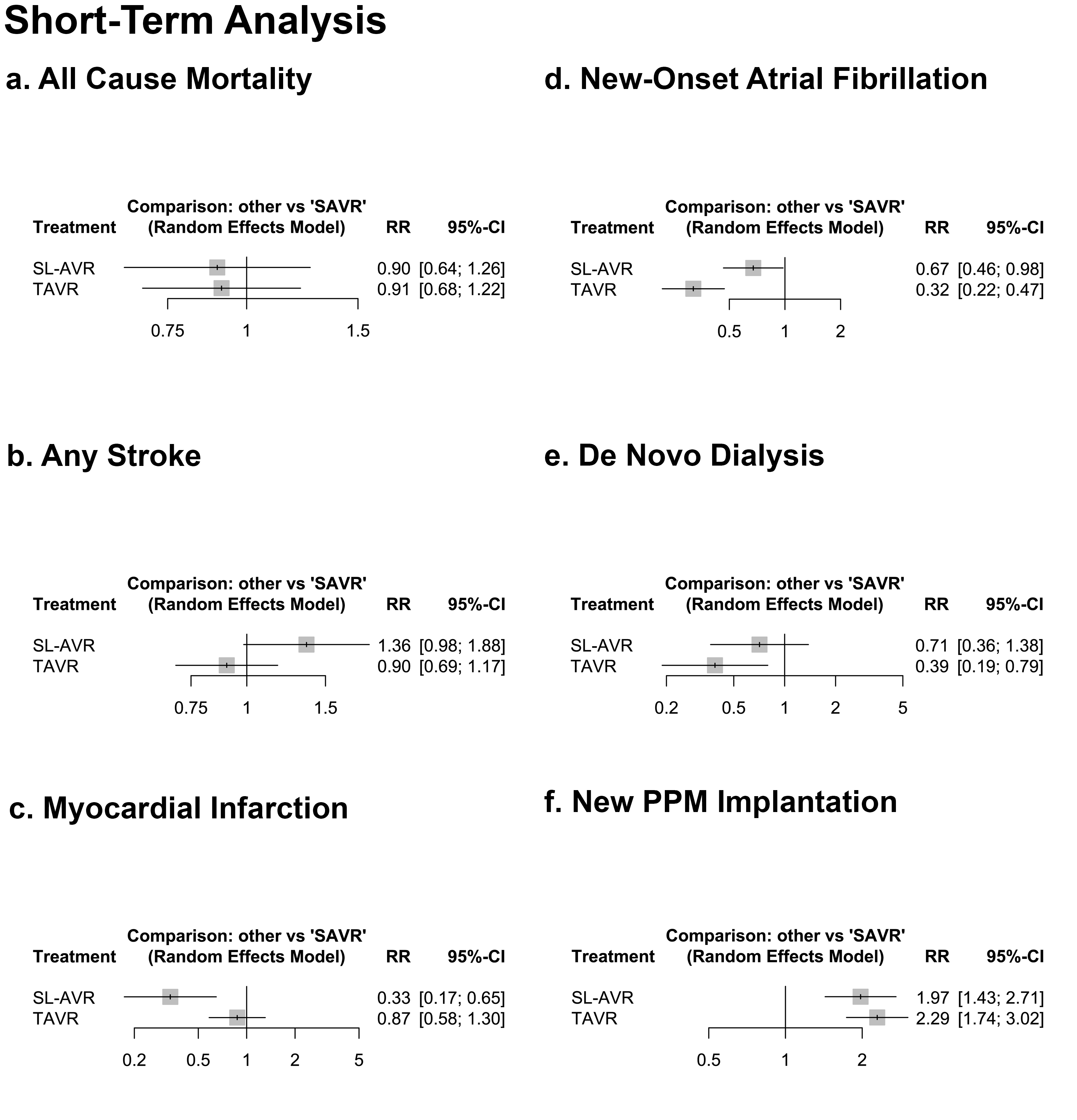
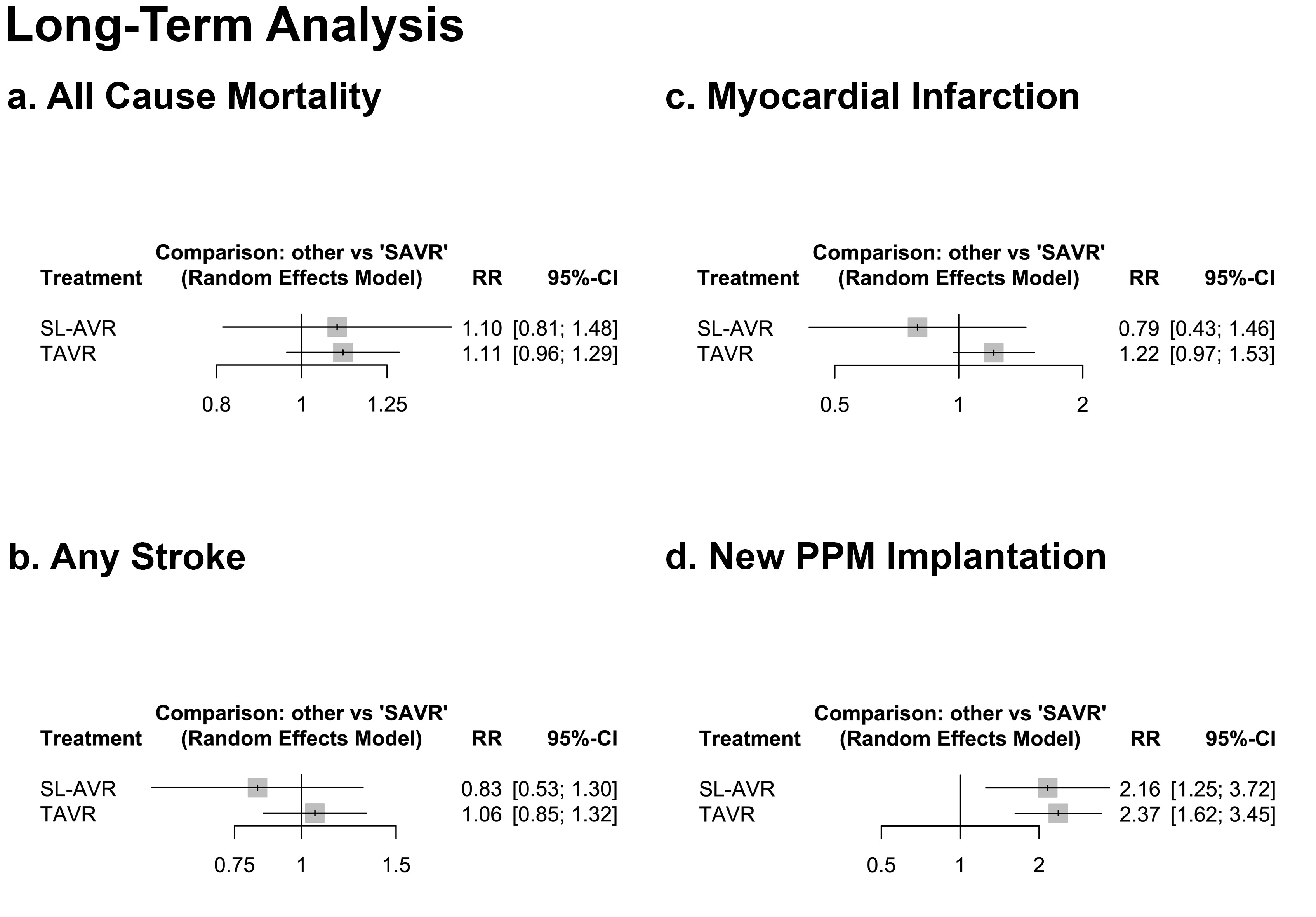
Comparative Outcomes of Transcatheter, Sutureless, and Surgical Aortic Valve Replacement in Patients With Low-to-Intermediate Surgical Risk: A Systematic Review and Network Meta-Analysis
By Bernadus Bernardino Bramantyo, Irene Yasmina Vilado, Naomi Natasha Napitupulu, Paulina Lusty Artanti, Bernardinus Prima Ardjie Pradipta, Khansa Maria, Pirel Aulia Baravia, Gerardo Kridanto Agung Laksono, Karina Yesika Manalu, Vanessa Carolina Gunawan, Koernia Kusuma Wardhana, Dyah Wulan Anggrahini, Lucia Kris Dinarti
Presenter
Authors
Affiliation
Comparative Outcomes of Transcatheter, Sutureless, and Surgical Aortic Valve Replacement in Patients With Low-to-Intermediate Surgical Risk: A Systematic Review and Network Meta-Analysis
Bernadus Bernardino Bramantyo1, Irene Yasmina Vilado2, Naomi Natasha Napitupulu1, Paulina Lusty Artanti3, Bernardinus Prima Ardjie Pradipta4, Khansa Maria1, Pirel Aulia Baravia5, Gerardo Kridanto Agung Laksono6, Karina Yesika Manalu7, Vanessa Carolina Gunawan8, Koernia Kusuma Wardhana9, Dyah Wulan Anggrahini1, Lucia Kris Dinarti1
Department of Cardiology and Vascular Medicine, Dr. Sardjito General Hospital, Yogyakarta, Indonesia1, Dr. Suhardi Hardjolukito Hospital, Bantul, Indonesia2, Oen Kandang Sapi Hospital, Solo, Indonesia3, Lavalette General Hospital, Malang, Indonesia4, Amanah Medical Center, Banjarmasin, Indonesia5, Department of Cardiothoracic and Vascular Surgery, Airlangga University, Surabaya, Indonesia6, Bhayangkara Hospital, Palangka Raya, Indonesia7, Faculty of Medicine, Brawijaya University, Malang, Indonesia8, Department of Cardiothoracic and Vascular Surgery, Saiful Anwar General Hospital, Malang, Indonesia9
Background
Methods
Results