Lots of interesting abstracts and cases were submitted for TCTAP 2026. Below are the accepted ones after a thorough review by our official reviewers. Don’t miss the opportunity to expand your knowledge!
ABS20251025_0001
Efficacy and Safety of Long-Time Pre-Dilation With Perfusion Balloon Prior to Stent Implantation in Acute Coronary Syndrome
By Kazuya Takihara, Keisuke Yamamoto, Makoto Takamatsu, Yasuhiro Honda, Kosuke Kadooka, Takeaki Kudo, Kenji Ogata, Toshiyuki Kimura, Kensaku Nishihira, Nehiro Kuriyama, Takashi Kubo, Nobuhiro Tanaka, Yoshisato Shibata
Presenter
Kazuya Takihara
Authors
Kazuya Takihara1, Keisuke Yamamoto2, Makoto Takamatsu2, Yasuhiro Honda2, Kosuke Kadooka2, Takeaki Kudo2, Kenji Ogata2, Toshiyuki Kimura2, Kensaku Nishihira2, Nehiro Kuriyama2, Takashi Kubo1, Nobuhiro Tanaka1, Yoshisato Shibata2
Affiliation
Department of Cardiology, Tokyo Medical University, Hachioji Medical Center, Tokyo, Japan1, Department of Cardiology, Miyazaki Medical Association Hospital, Miyazaki, Japan2
View Study Report
ABS20251025_0001
ACS/AMI
Efficacy and Safety of Long-Time Pre-Dilation With Perfusion Balloon Prior to Stent Implantation in Acute Coronary Syndrome
Kazuya Takihara1, Keisuke Yamamoto2, Makoto Takamatsu2, Yasuhiro Honda2, Kosuke Kadooka2, Takeaki Kudo2, Kenji Ogata2, Toshiyuki Kimura2, Kensaku Nishihira2, Nehiro Kuriyama2, Takashi Kubo1, Nobuhiro Tanaka1, Yoshisato Shibata2
Department of Cardiology, Tokyo Medical University, Hachioji Medical Center, Tokyo, Japan1, Department of Cardiology, Miyazaki Medical Association Hospital, Miyazaki, Japan2
Background
We sought to investigate the efficacy and safety of long-time pre-dilation with perfusion balloon prior to stent implantation as compared to direct stenting in percutaneous coronary intervention (PCI) for acute coronary syndrome (ACS). Perfusion balloon, which enables long-time pre-dilation by maintaining coronary blood flow, is expected to enhance thrombus/plaque compression and promote lesion dilation during PCI.
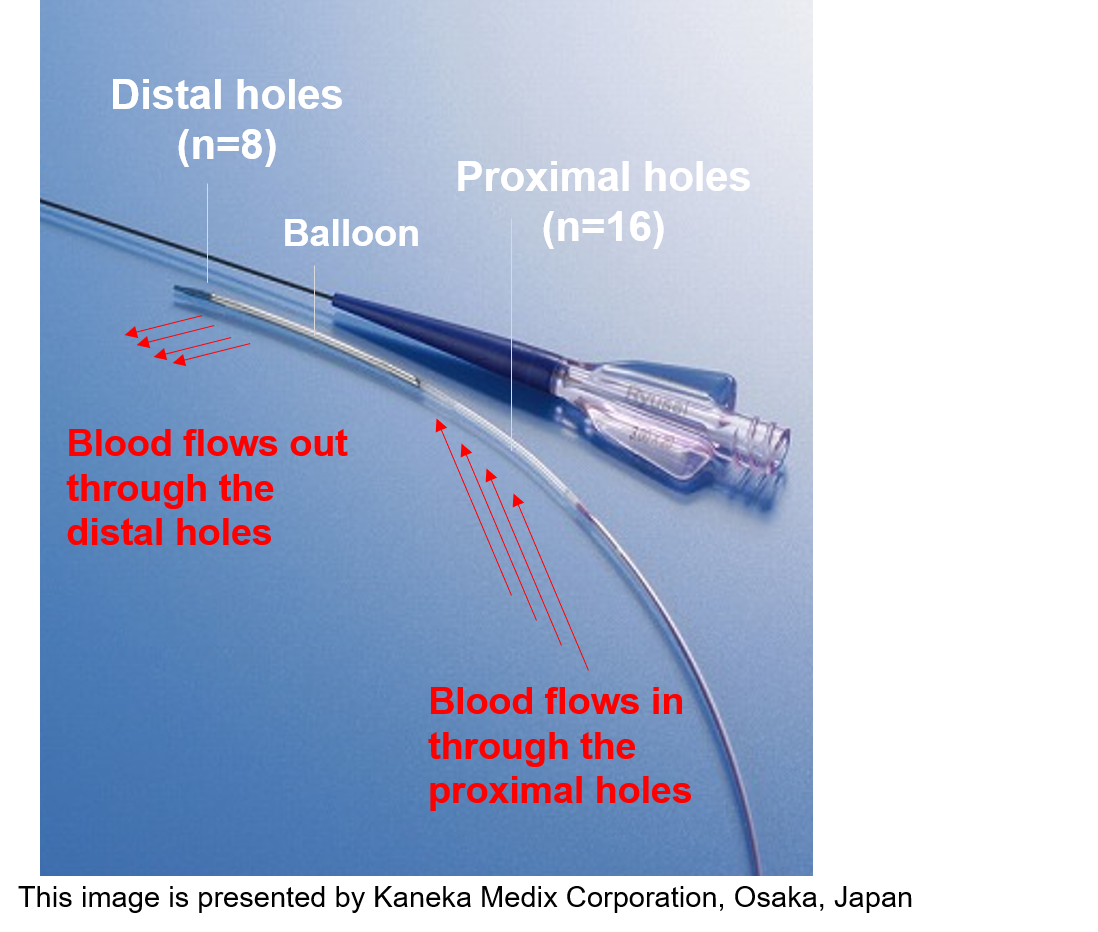

Methods
We studied 117 ACS patients who underwent PCI with long-time pre-dilation using a perfusion balloon (Ryusei, Kaneka Medix Corporation, Osaka, Japan) prior to stent implantation (n = 55) or direct stenting (n = 62). The findings of angiography and intravascular imaging at post-PCI, as well as major adverse cardiovascular events (MACE: defined as a composite of cardiac death, myocardial infarction, or clinically-driven target lesion failure) at one-year follow-up, were compared between the two groups.
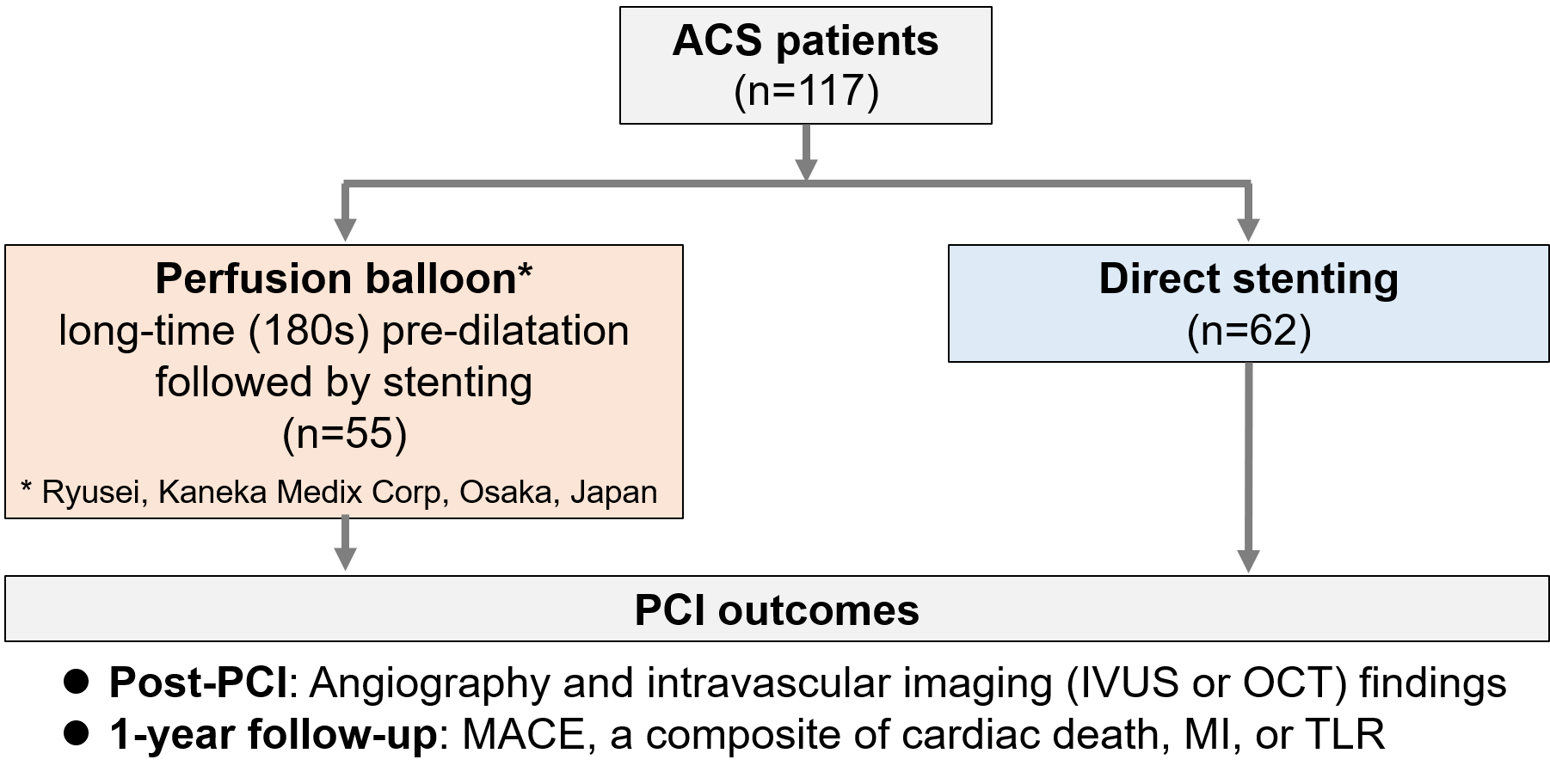

Results
Patient and lesion characteristics at baseline were not different between the two groups. For pre-dilation, perfusion balloon diameter was 3.0 mm (interquartile range [IQR]: 3.0–3.0 mm) and perfusion balloon inflation time was 180 sec (IQR: 120–180 sec). Stent diameter and frequency of post-dilation balloon use were comparable between the two groups. Minimum stent area was similar between the two groups. Minimum intra-stent lumen area was significantly larger in the perfusion balloon pre-dilation group than the direct stenting group (6.27 mm2 [IQR:5.38–7.48 mm2] vs. 5.90 mm2 [IQR: 4.85–6.79 mm2],p = 0.024). The frequency of irregular thrombus/plaque protrusion was significantly lower in the perfusion balloon pre-dilation group than the direct stenting group (7.3% vs. 45.2%, p < 0.001). Maximum thrombus/plaque protrusion area was significantly smaller in the perfusion balloon pre-dilation group than the direct stenting group (0.00 mm2 [IQR:0.00–0.42 mm2] vs. 0.46 mm2 [IQR: 0.00–1.07 mm2],p = 0.021). There was no difference between the two groups in the frequency of slow flow/no reflow and distal embolization during PCI, nor in the frequency of MACE at one-year follow-up.

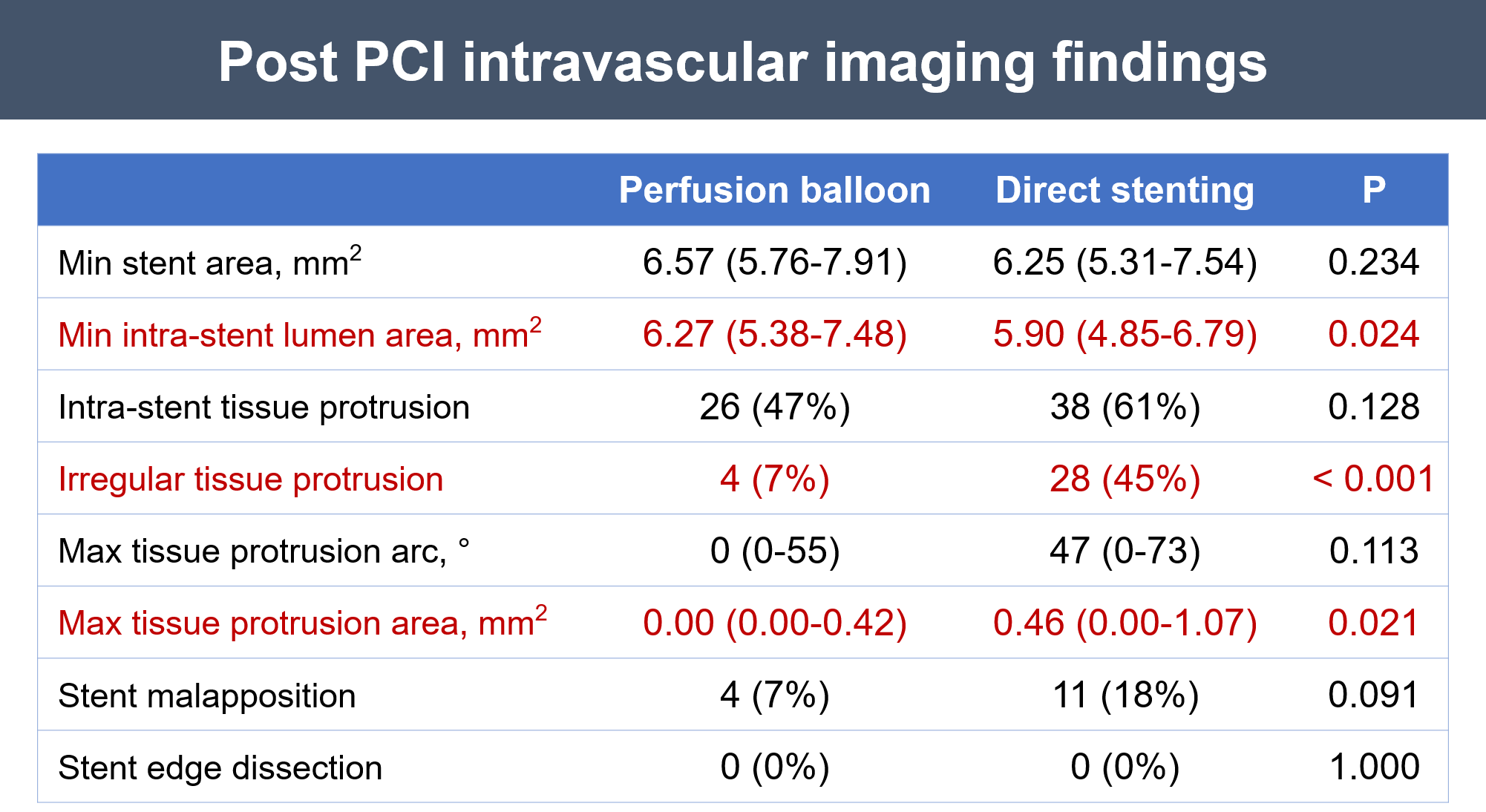




Conclusion
In PCI for ACS, the long-time pre-dilation with a perfusion balloon prior to stent implantation, compared to direct stenting, resulted in a larger intra-stent lumen area by reducing irregular thrombus/plaque protrusion without increasing slow flow/no reflow and distal embolization.
