Lots of interesting abstracts and cases were submitted for TCTAP 2026. Below are the accepted ones after a thorough review by our official reviewers. Don’t miss the opportunity to expand your knowledge!
ABS20251002_0002
National Reimbursement Policy and Its Impact on Risk Profile and Clinical Outcomes in Transcatheter Aortic Valve Implantation
By Weiting Wang, Hsiao-Huang Chang, I-Min Chen, Yin-Hwa Chen
Presenter
Weiting Wang
Authors
Weiting Wang1, Hsiao-Huang Chang1, I-Min Chen2, Yin-Hwa Chen2
Affiliation
Taipei Veterans General Hospital, Taiwan1, Taipei Veterans General Hospital , Taiwan2
View Study Report
ABS20251002_0002
Other Structural Interventions
National Reimbursement Policy and Its Impact on Risk Profile and Clinical Outcomes in Transcatheter Aortic Valve Implantation
Weiting Wang1, Hsiao-Huang Chang1, I-Min Chen2, Yin-Hwa Chen2
Taipei Veterans General Hospital, Taiwan1, Taipei Veterans General Hospital , Taiwan2
Background
Background: Transcatheter aortic valve implantation (TAVI) is an established treatment for severe aortic stenosis . While reimbursement policies significantly expand access, the impact of Taiwan's National Health Insurance (NHI) coverage introduced in February 2021 on patient characteristics and outcomes remains unclear. This study evaluates changes in patient profiles, and clinical outcomes before and after NHI reimbursement.
Methods
Methods : We analyzed 467 patients undergoing TAVI at a high-volume tertiary center between May 2010 and April 2024. Patients were divided into pre-reimbursement (n=258) and post-reimbursement (n=209) groups. P atient profiles , procedural variables, and clinical outcomes , including 30-day complications and 1-year all-cause mortality, cardiovascular death, and rehospitalization for heart failure (HF) , were compared. Risk was stratified using the Society of Thoracic Surgeons (STS) score.
Results
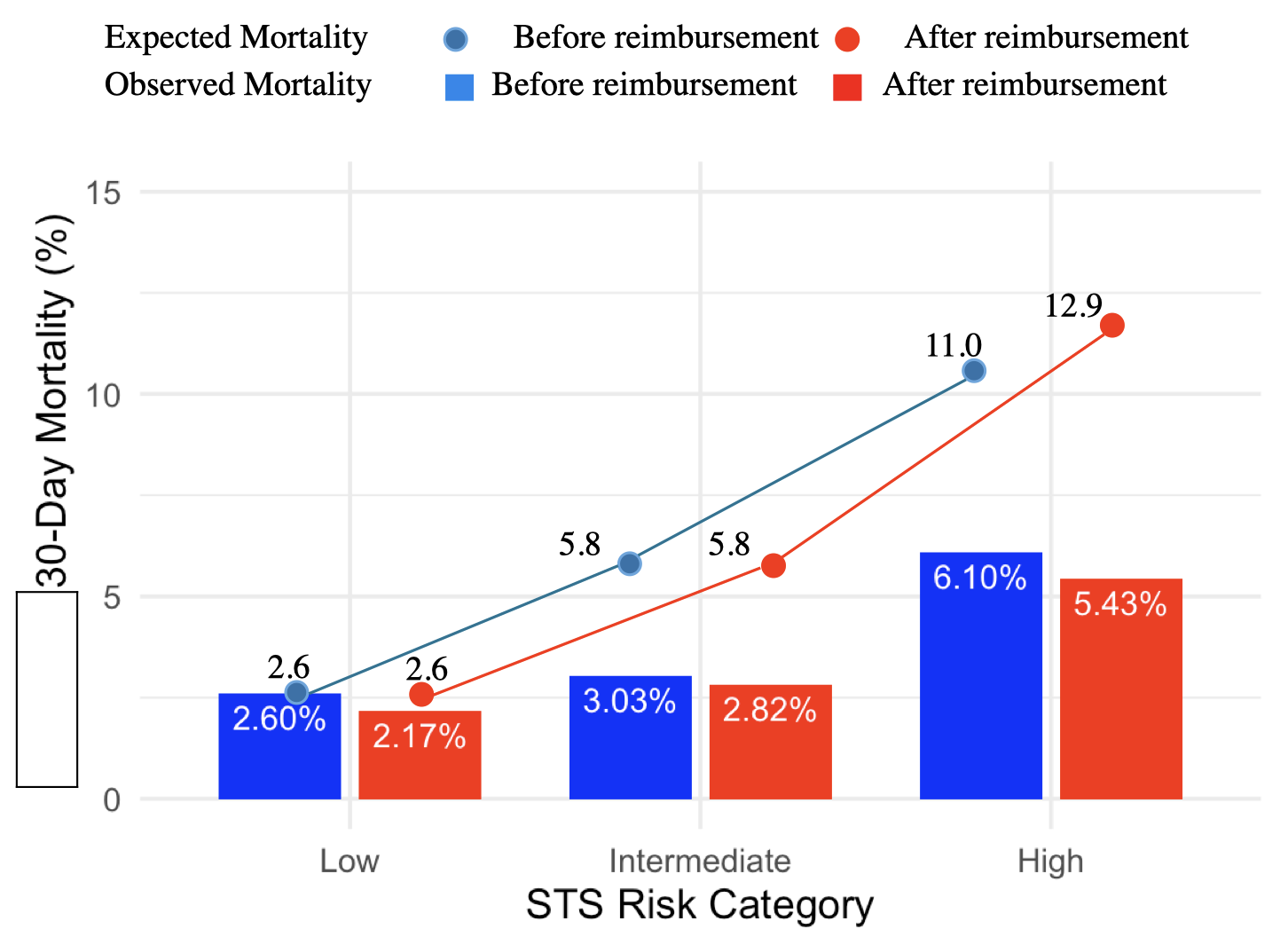
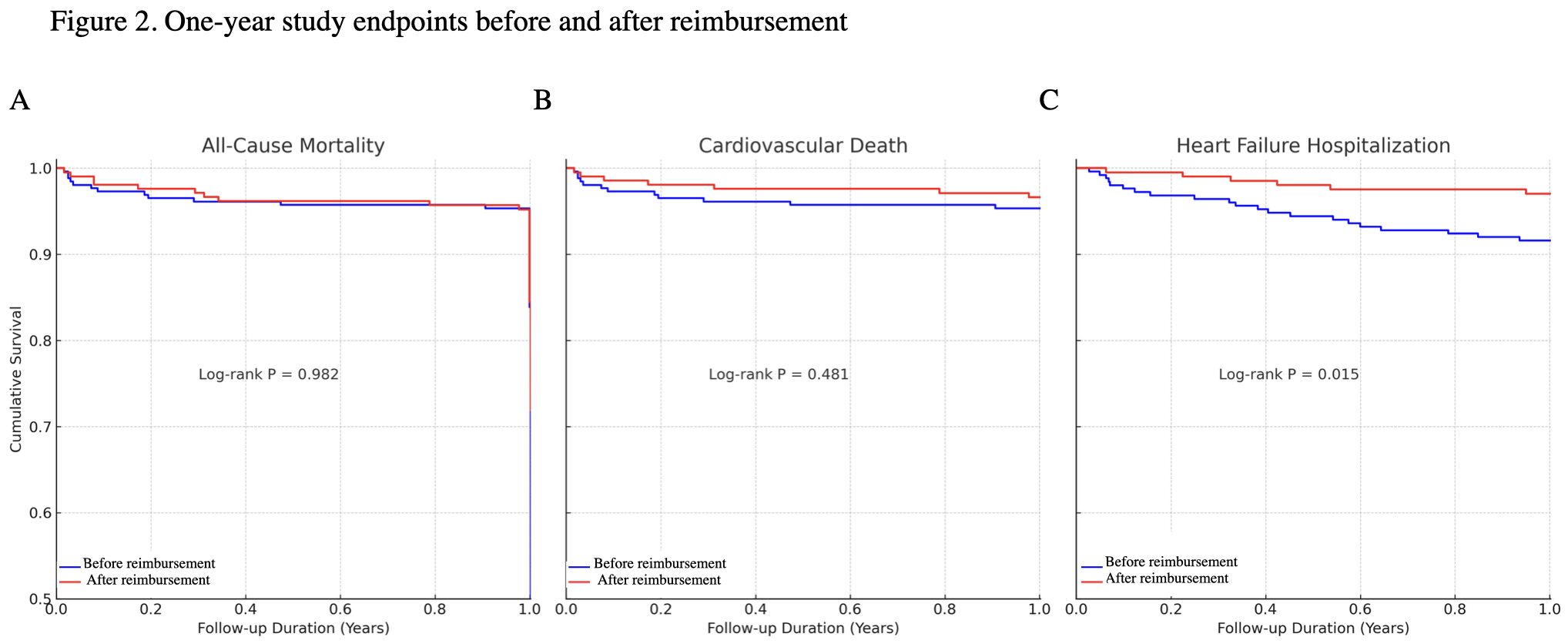
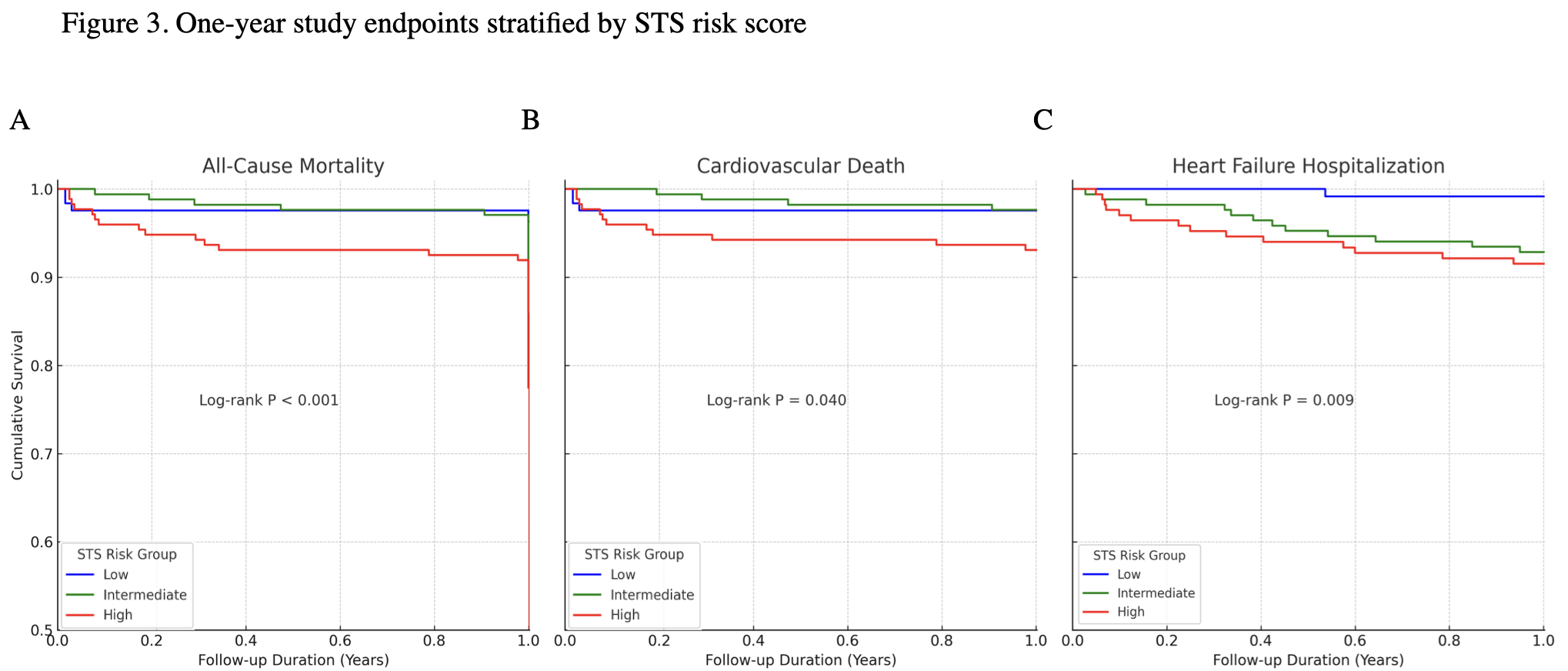
Results: Reimbursement was associated with a shift toward higher-risk patients, reflected by an increase in median STS scores (5.9% to 7.2%, p=0.002) and more patients classified as high-risk (44.0% vs. 31.8%, p=0.019). Post-reimbursement patients had higher frequency of dialysis (17.7% vs. 7.6%, p=0.001) and valve-in-valve procedures (8.4% vs. 2.7%, p=0.007), but shorter hospital stays (7.0 vs. 10.0 days, p<0.001). VARC-3 defined thirty-day outcomes were similar, except for reduced acute kidney injury in post-reimbursement patients (1.0% vs. 6.6%, p=0.021). One-year mortality was unchanged, but HF rehospitalization decreased significantly (2.9% vs. 8.1%, p=0.017). After multivariable adjustment, high STS risk (≥8%) independently predicted worse one-year outcomes.
TAVI Figure 1.png
TAVI Figure 2.png
TAVI Figure 3.png

TAVI Figure 1.png

TAVI Figure 2.png

TAVI Figure 3.png
Conclusion
Conclusion: NHI reimbursement in Taiwan expanded TAVI access to higher-risk patients without compromising short- or mid-term mortality, and was associated with improved heart failure readmission, especially among high-risk patients.
