Lots of interesting abstracts and cases were submitted for TCTAP 2026. Below are the accepted ones after a thorough review by our official reviewers. Don’t miss the opportunity to expand your knowledge!
ABS20250911_0001
Beyond the Stent : Adverse Risk Predictors and Outcomes of PCI – A Cohort Study From Sri Lanka
By Mohamed Basheer Fasllur Rahuman, Nimali Fernando, Chathurika Kempitiya, Anushka Peiris, Pasan Abeysenevi, Leonard Wanninayake, Reeni Robert, Chirani Ratnayake, Amanda Nawarathna, Pubudu De Silva
Presenter
Mohamed Basheer Fasllur Rahuman
Authors
Mohamed Basheer Fasllur Rahuman1, Nimali Fernando1, Chathurika Kempitiya1, Anushka Peiris1, Pasan Abeysenevi1, Leonard Wanninayake1, Reeni Robert1, Chirani Ratnayake1, Amanda Nawarathna1, Pubudu De Silva2
Affiliation
National Hospital of Sri Lanka, Sri Lanka1, Ministry of Health, Sri Lanka2
View Study Report
ABS20250911_0001
ACS/AMI
Beyond the Stent : Adverse Risk Predictors and Outcomes of PCI – A Cohort Study From Sri Lanka
Mohamed Basheer Fasllur Rahuman1, Nimali Fernando1, Chathurika Kempitiya1, Anushka Peiris1, Pasan Abeysenevi1, Leonard Wanninayake1, Reeni Robert1, Chirani Ratnayake1, Amanda Nawarathna1, Pubudu De Silva2
National Hospital of Sri Lanka, Sri Lanka1, Ministry of Health, Sri Lanka2
Background
This study aimed to analyze percutaneous coronary intervention (PCI) patterns and outcomes in Sri Lanka to better understand patient trends post-PCI and contribute to improving the management of coronary artery disease (CAD).
Methods
A prospective single-center cohort study was conducted among all 758 patients who underwent PCI in Unit 2 of the National Heart Center, Sri Lanka during February 2022 and December 2023. Clinical patterns, risk factors, management strategies, and post-PCI outcomes were studied. They were followed up in-hospital, at 1, 3 and 6 months. Selection bias was reduced by including all consecutive patients who underwent PCI during our study period, ensuring comprehensive and unbiased enrollment. 89 patients (11.7%) were lost to follow up at 6 months for outcome analysis and excluded from the study.Ethical clearance was obtained from the Ethics Review Committee of the institution. Patients or the public were not involved in defining research questions, study design and evaluation of outcomes. Informed consent was taken from all the participants in this study.


Results
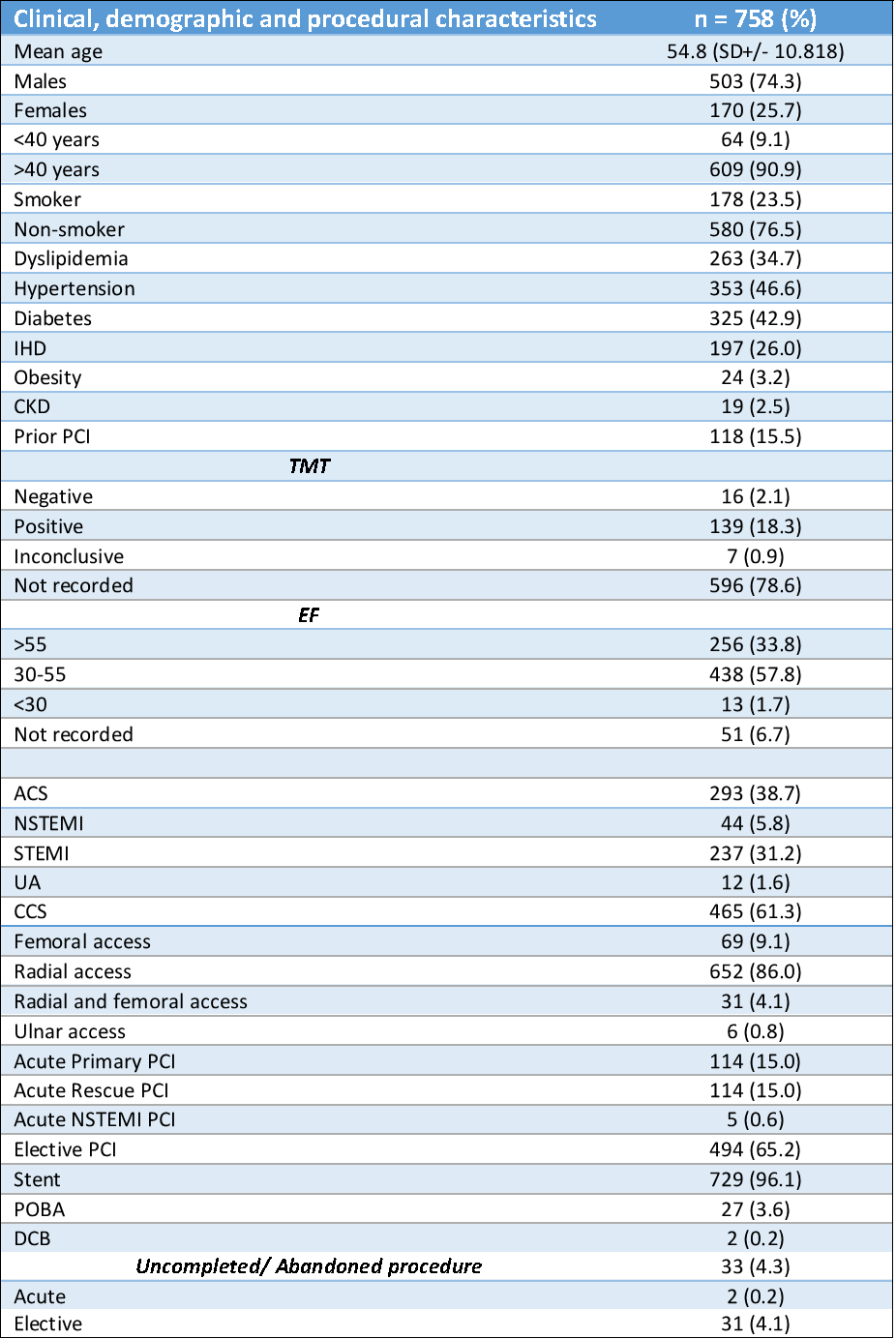
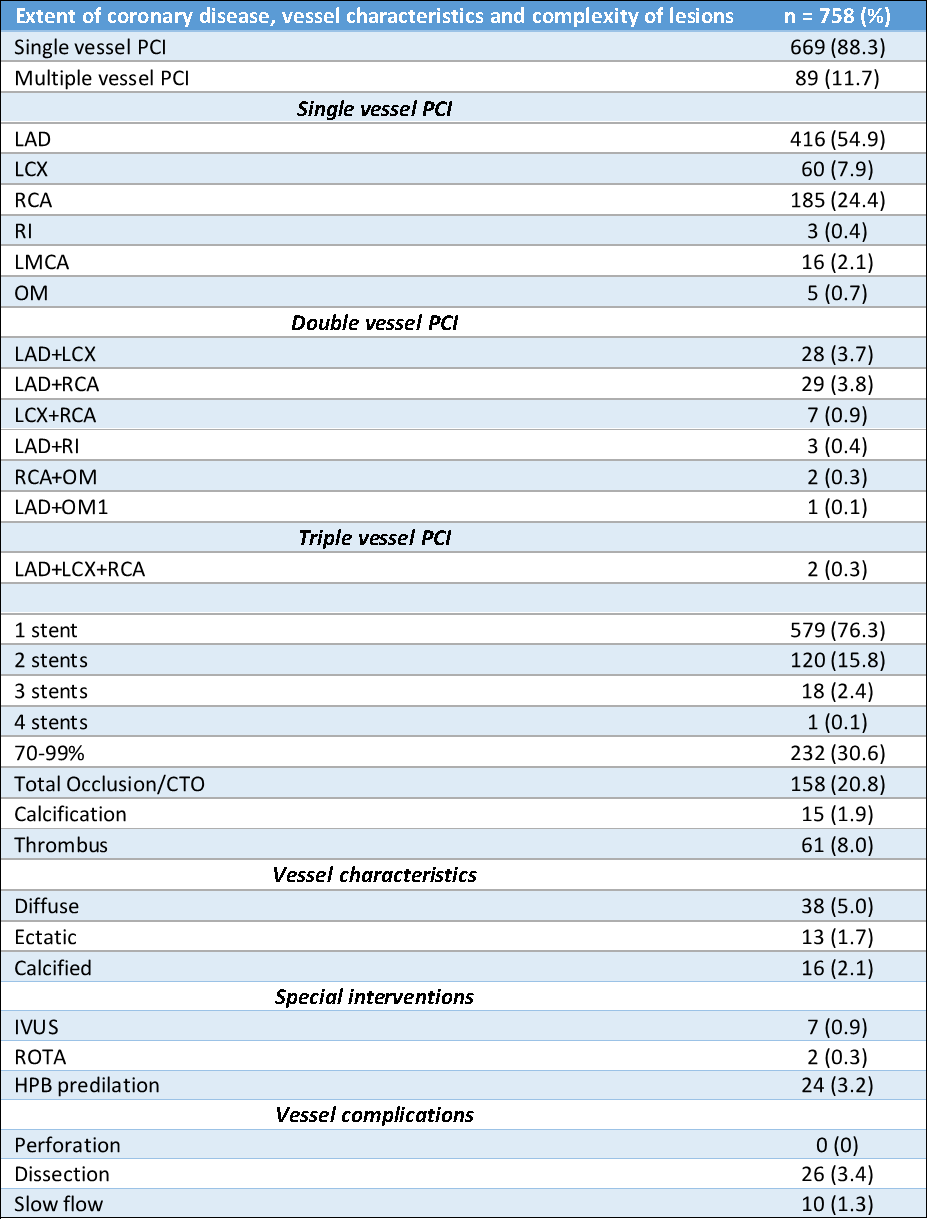
The mean age of participants was 54.8 years (SD±10.8), with 74.3% being male and 90.9% aged over 40. Hypertension and diabetes were the most prevalent risk factors. Prior PCI was reported in 15.5% of patients, and 57.8% had an ejection fraction (EF) between 30–55%. Chronic coronary syndrome (CCS) was the most common presentation (61.3%), while 38.6% had acute coronary syndrome (ACS) of which 31.2% presented with ST-elevation myocardial infarction (STEMI). Radial access was achieved in 86% of cases, 30.7% received acute PCI and 69.3% underwent elective PCI. Single-vessel PCI was performed in 88.3%, with the left anterior descending artery (LAD) being the most frequently stented vessel (54.9%). Chronic total occlusions (CTOs) were found in 20.8%. The procedural success rate was 94.6%. In-hospital mortality was 0.79%, and six-month mortality was 2.5%. Hypertension and EF <30% were independent predictors of adverse outcomes.
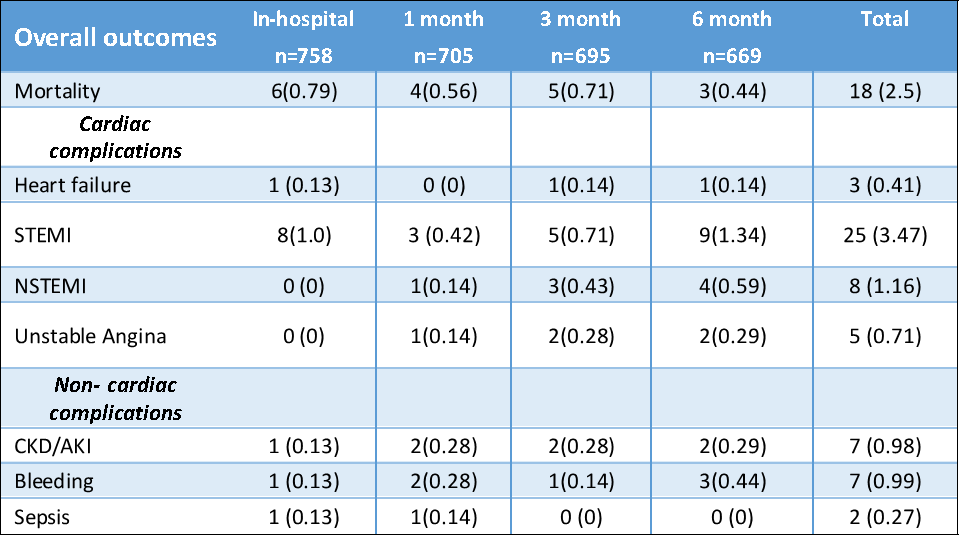
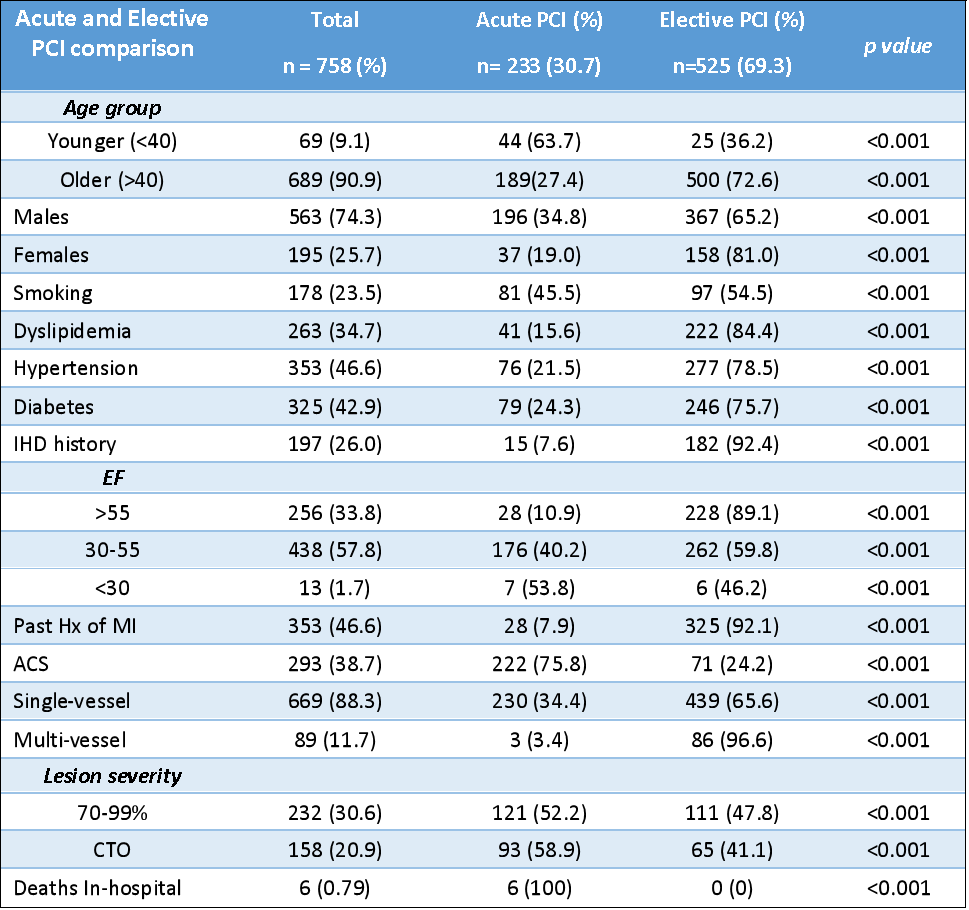
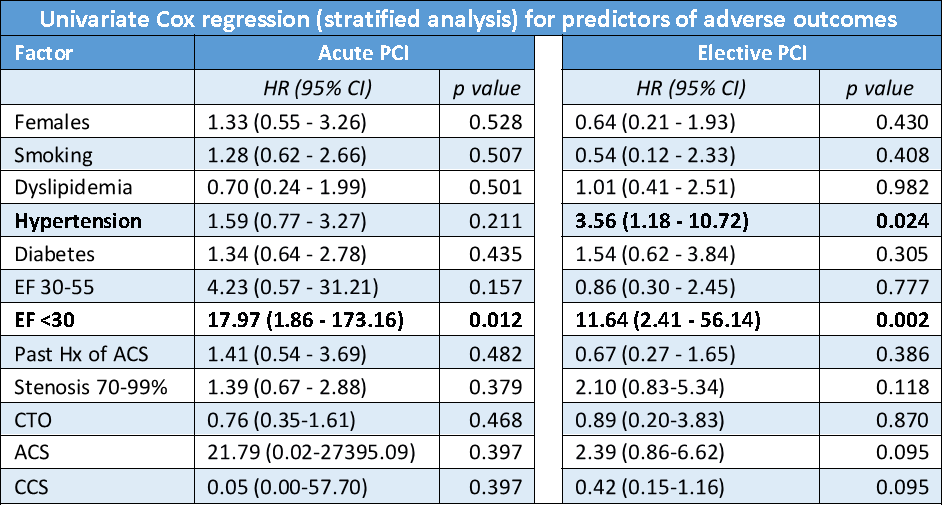



Conclusion
Our research provides novel insights into the characteristics and outcomes of patients who have undergone PCI in Sri Lanka. The key risk factors were identified as hypertension and diabetes. A procedural success rate of 94.6% was observed in our study. The univariate cox regression analysis revealed that the critical predictors of adverse outcomes post-PCI were EF<30 in the acute PCI group and hypertension and EF<30 in the elective PCI group, underscoring the importance of targeted interventions and monitoring in this population. Despite the resource-poor settings and economic constraints in the South Asian region, we observed favorable outcomes, with an in-hospital mortality rate of 0.79% and a 6-month mortality rate of 2.5%, which are notable when compared with findings from regional studies.All these findings emphasize the need for tailored clinical strategies to further improve patient outcomes and inform future research and healthcare policies in Sri Lanka. Continued efforts to address identified risk factors may enhance the overall effectiveness of PCI and contribute to better long-term survival rates.